Australian man’s HR meeting leads to frontotemporal dementia diagnosis
A 54-year-old IT veteran’s performance-review ordeal exposes how younger-onset dementia can emerge under the radar and stress the need for proactive, tailored support.
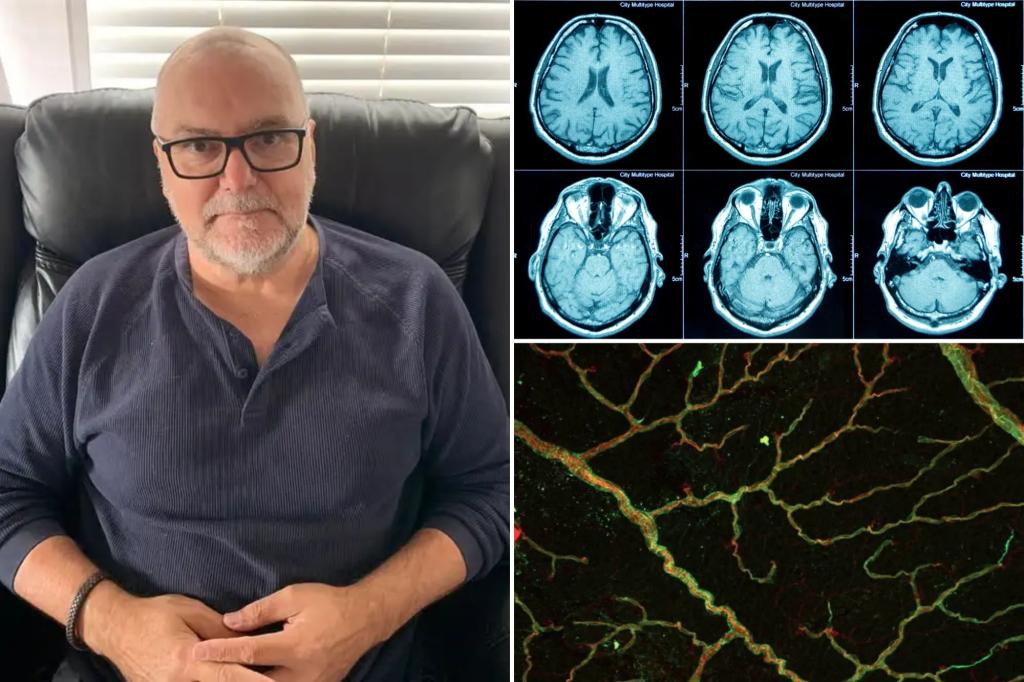
Patrick Dare, a 54-year-old Australian IT sales veteran, was called into his first human resources review, a moment that would reshape his life. After years of steady performance, he began experiencing mood changes and escalating anger that were out of character. What started as irritability in the evenings progressed to paranoia and culminated in a public outburst that prompted the HR meeting. Following a battery of tests, Dare was diagnosed in 2019 with frontotemporal dementia, a form of dementia that can strike people well before traditional retirement age.
Before the diagnosis, Dare had already survived a bout of depression in 2006. He initially worried the symptoms signaled another mental-health episode, but doctors pointed to a neurodegenerative condition that disrupts brain networks governing behavior. Associate Professor Rowena Mobbs, a leading dementia physician, notes that frontotemporal dementia can manifest as Behavioral and Psychological Symptoms in Dementia, or BPSD, which may include mood swings, aggression, and social withdrawal. BPSD raises the risk of falls, hospitalizations, delirium, and overmedication, but early detection can help people live more safely in the community and relieve caregiver burden. Dare described the moment of diagnosis as both shocking and a relief: it finally explained the misfiring moments and opened a path to address them, including strategies to curb inappropriate behavior.

More than 433,000 Australians are living with dementia, and AIHW projections indicate the number could rise to about one million by 2065. Within that group, roughly 29,000 people are under 65, with younger-onset dementia expected to grow about 41 percent to around 41,000 by 2054. Tim England of YOD Reflections, which supports people with younger-onset dementia, warned that at the current rate a new younger-onset dementia diagnosis will occur every day for three decades. “For a lot of our clients, they’re grappling with a diagnosis while still trying to pay a mortgage, raise kids, and manage school runs,” England said. He compared the current system’s gaps to the care pathways that exist for breast cancer patients, where navigators help people access services and keep care coordinated. Mobbs supported the broader point, noting that people with dementia often lack a structured, proactive support system that can ease the burden on families. The Think Again campaign, backed by News.com.au and The Australian, has highlighted how dementia messaging and services can lag behind other illnesses.
For Dare, the diagnosis brought a bittersweet clarity. He remained employed until 2021, but the technical demands of the job eventually proved overwhelming. The transition away from a longtime career hit him hard, but he chose to turn his experience into advocacy. Today he sits on Dementia Australia’s Advisory Committee and speaks publicly about how younger-onset dementia can allow for meaningful, independent lives with the right planning and supports. He describes his brain as “a duck on the surface,” sailing smoothly while the legs beneath tirelessly paddle to keep him steady. He has learned to regulate his activities, avoiding late nights and afternoon driving, and he works to acknowledge and explain lapses when they occur. When asked about his former colleagues, Dare smiles at the memory and says they still meet for coffee, even joking about his “dementia card.”
The path Dare has chosen reflects a broader push to rethink how health systems respond to dementia in younger people. While his experience underscores the human dimension of the illness, it also spotlights the need for earlier detection, tailored support services for younger patients, and integrated care that spans medical treatment, counseling, and family planning. Advocates argue that giving people a navigable pathway—akin to the support offered to breast cancer patients—could reduce isolation and help families plan for long-term care.
In the wake of Dare’s story, health experts emphasize that dementia is not solely about memory loss. Frontotemporal dementia, in particular, often targets behavior and personality before memory, presenting a unique set of challenges for patients, families, and workplaces. The condition’s rising prevalence among younger adults is prompting calls for workplace education, early screening, and community resources that acknowledge the distinct needs of younger patients and their families. As Dare continues to share his journey, he hopes to illuminate paths to independence, reduce stigma, and spur concrete reforms that equip people with dementia to live with dignity and purpose.