CDC: 'Nightmare' drug-resistant bacteria rising in the U.S.; NDM gene drives surge
CDC reports a 70% rise in infections involving the NDM gene between 2019 and 2023, but testing gaps likely undercount cases; experts warn of grave danger as resistant infections spread.
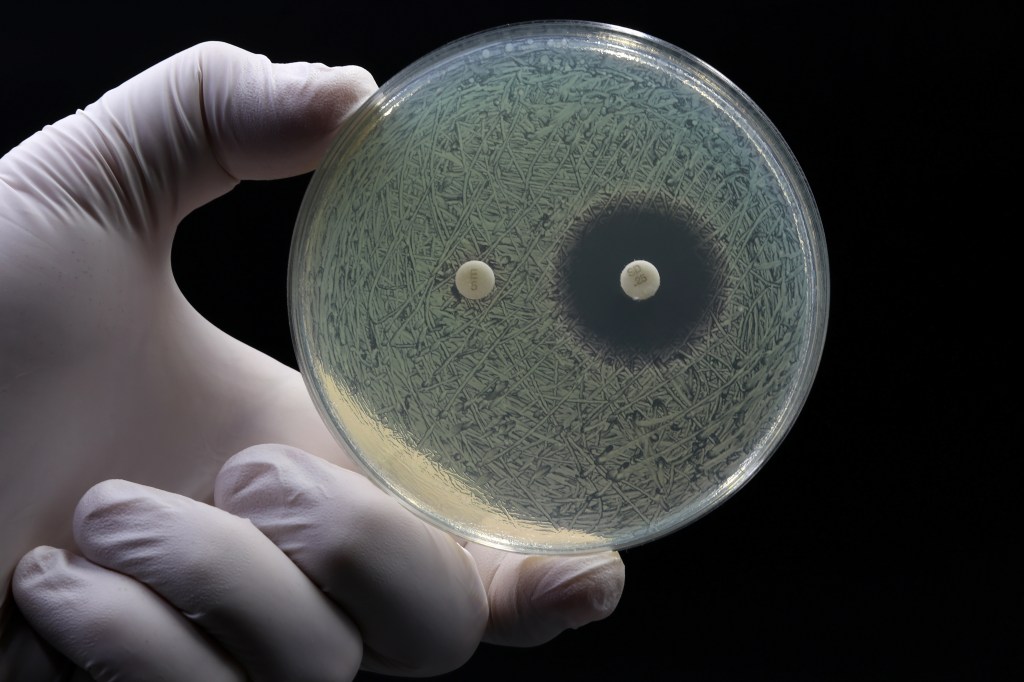
A Centers for Disease Control and Prevention analysis released this week shows a growing threat from drug-resistant bacteria in the United States, including bacteria labeled as “nightmare” pathogens because they resist many antibiotics. The report finds that infections caused by carbapenem-resistant organisms rose 69% from 2019 to 2023, and infections carrying the NDM gene surged even more sharply over the same period. Across 29 states, health officials counted 4,341 carbapenem-resistant infections in 2023, of which 1,831 involved the NDM gene.
Two antibiotics can treat NDM-related infections, but they must be given intravenously and are expensive. The bacteria carrying the NDM gene were once considered exotic and confined to small, overseas outbreaks, but they are now appearing in the United States with increasing frequency. Although the total number of NDM cases remains relatively small, the rise in cases over the past several years has been striking. The study’s authors cautioned that the total nationwide burden is likely higher than the numbers show because of gaps in testing and reporting across states.
Experts emphasize that routine infections seen in clinics and hospitals—such as urinary tract infections and wound infections—could become more difficult to treat if caused by NDM-positive organisms. The rise aligns with broader concerns about antimicrobial resistance, a phenomenon that occurs when germs evolve to withstand the drugs designed to kill them. Scientists underscore that the misuse of antibiotics—such as not completing prescribed courses or seeking antibiotics for viral illnesses—fuels resistance and complicates treatment decisions.
The CDC highlighted that the rate of carbapenem-resistant infections increased from just under 2 infections per 100,000 people in 2019 to more than 3 per 100,000 in 2023, a 69% rise. The rate of NDM-carrying infections alone exploded from around 0.25 per 100,000 to about 1.35 per 100,000, a roughly 460% increase, according to the agency’s analysis. The numbers reflect 29 states reporting data in 2023, and the researchers noted that the trend likely understates the true scope because testing for genetic resistance varies by facility and state.
The CDC’s estimates do not fully capture all major states, including California, Florida, New York, and Texas, where reporting and testing practices differ. A June CDC update also noted an uptick in NDM cases in New York City between 2019 and 2024, underscoring the potential for broader community spread if carriers remain undetected. Health officials say asymptomatic carriers may carry the bacteria without obvious signs, which could allow transmission in households, workplaces, and healthcare settings.
Experts cautioned that the pandemic-era surge in antibiotic use may have contributed to the rise in resistant infections. Dr. Jason Burnham, a researcher at Washington University, said in an interview that the broad increase in antibiotic consumption during the COVID-19 era likely exerted selective pressure that favors resistant strains. He stressed that multiplying testing capacity and improving reporting are essential to understanding and curbing the spread.
"The rise of NDMs in the U.S. is a grave danger and very worrisome," said David Weiss, an infectious diseases researcher at Emory University, in an email. Weiss noted that many people who harbor resistant bacteria may not show symptoms, which could enable hidden transmission in communities as well as healthcare facilities.
Health officials emphasize that while the current number of infections is still relatively small in the context of the U.S. population, the trajectory matters for patient safety and hospital preparedness. The panel of experts cited the need for strengthened antimicrobial stewardship, expanded surveillance, and investment in diagnostic testing that can rapidly identify genetic resistance in bacteria.
For patients, the development translates into longer, more complicated illnesses and higher health care costs. If a standard infection such as a urinary tract infection is caused by a carbapenem-resistant organism, doctors may need to resort to last-resort therapies that are less effective, more toxic, or both. Hospitals must balance infection-control measures, such as isolation protocols and environmental cleaning, with the realities of patient load and resource constraints.
The CDC and other public health groups say the fight against antimicrobial resistance requires a coordinated approach: prudent antibiotic prescribing, rapid diagnostic tests, better reporting, and ongoing research into new and combination therapies. While the current numbers demonstrate a troubling trend, officials stress that prompt action at the clinical, local, and national levels can help slow the spread and protect patients from infections that are harder to treat.
As investigators continue to refine estimates and fill gaps in surveillance, health care providers are urged to maintain strict infection-control practices and to educate patients about the importance of completing prescribed antibiotic courses and avoiding the inappropriate use of antibiotics. The public should understand that antimicrobial resistance is a dynamic, long-term threat that requires sustained attention and resources to prevent a future in which common infections become disproportionately dangerous.