Coroner warns of fatal VBAC risks not disclosed after newborn's death
Inquest finds lack of warning about uterine rupture after previous cesarean and urges review of antenatal guidance and leaflets.
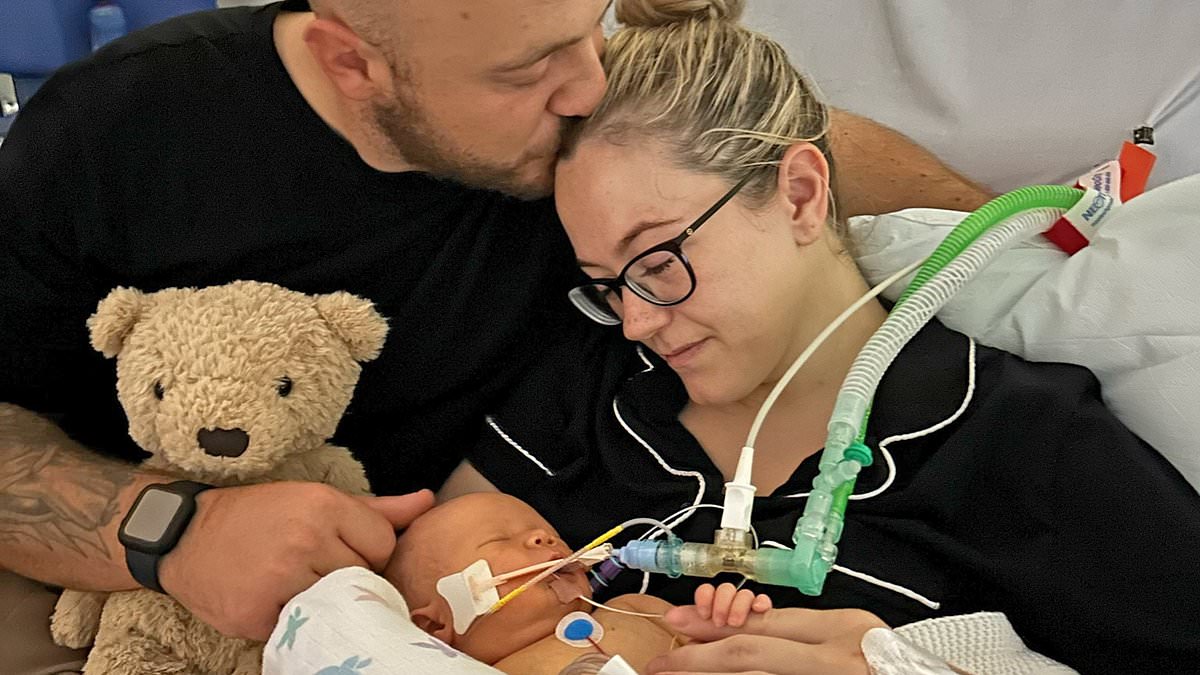
Swindon, England — A coroner has warned that pregnant women are not being told of the potentially fatal risks of vaginal birth after cesarean, following the death of a newborn girl.
Mabel Williams, who died at six days old from brain injuries caused by a lack of oxygen during birth, is at the center of an inquest that found her mother experienced an undiagnosed uterine rupture after a vaginal birth after cesarean (VBAC). Becky Williams, 34, an office manager from Swindon, Wilts, had been told VBAC could lead to uterine rupture but was not informed of the fatal risks associated with the option. The inquest heard midwives failed to recognise multiple indicators of Mabel’s distress and to convey the worsening condition of Becky Williams to the clinical team, according to the coroner’s findings.
During the birth at Swindon’s Great Western Hospital, the birth was induced and synthetic oxytocin was used, with researchers noting that Becky Williams had not been warned that this could further increase the risk of rupture. Mabel died six days later on Sept. 10, 2023. The coroner, Robert Sowersby, has issued a Prevention of Future Deaths (PFD) report following the death and has called for a review of antenatal care and the information provided to pregnant women considering VBACs.
My concern is that prospective parents may rely on this information leaflet to assist them in making informed choices about their birth options, and that if the risk is not identified, then other patients like Becky might pursue VBAC in circumstances where – if they had understood the risk better – they would have chosen otherwise, Sowersby wrote in the PFD. He noted that revised leaflets containing a fuller explanation of uterine rupture had been drafted but were not signed off by the NHS Trust for distribution to patients, which frustrated the maternity unit.
The inquest highlighted that the information leaflet produced by the Royal College of Obstetricians and Gynaecologists (RCOG) – titled Birth options after previous caesarean section and published in July 2016 – did not indicate that a uterine rupture could be fatal for either mother or baby. When Becky Williams was advised about VBAC, she was referred to both hospital internal guidance and the RCOG leaflet, neither of which clearly warned of the potential fatal consequences. The inquest pointed to what it described as neglect by the NHS that contributed to Mabel’s death.
In a statement, Becky and Tom Williams, Mabel’s parents, said: “We’re grateful that the Coroner has issued Prevention of Future Deaths reports to both the Trust and the Royal College of Obstetricians and Gynaecologists following Mabel’s inquest. The findings confirm what we have always known, that Mabel’s death was avoidable. Nothing will bring our daughter back, but these reports must now lead to visible change. We expect a transparent action plan with deadlines, not just acknowledgments. We will keep speaking Mabel’s name and pushing for improvements so that no other family endures what we have.”
Amy Milner, a senior associate at CL Medilaw representing Becky and Tom Williams, welcomed the coroner’s decision to alert the RCOG and the Trust to concerns about current guidance for birth after cesarean. Milner said the inquest showed that clinicians had not ensured Becky understood the significant implications a uterine rupture could have for both her and Mabel, and that the leaflets did not explain that rupture can be fatal or describe its consequences. Milner emphasized the need for proper communication about VBAC risks and careful labor management to reduce rupture risk, adding that Mabel’s case illustrates why updated guidance is vital to prevent further loss of life.
The coroner’s PFD to the hospital and to the RCOG calls for a formal review of the information given to expectant mothers considering VBACs and for clear, unequivocal language about the risk of uterine rupture and its potentially fatal outcomes. It also underlines the necessity of ensuring that revised patient information is approved and distributed to patients, rather than remaining in draft form. The NHS Trust and the RCOG were urged to implement an action plan with timelines to improve antenatal counseling and to ensure labour is monitored to minimize rupture risk. The inquest and the subsequent PFDs highlight broader questions about how birth options after cesarean are presented to patients and how frontline staff convey risk information.
The case has drawn attention to an ongoing debate over VBAC safety and patient consent. Proponents of VBAC argue that many women who have had a prior cesarean can safely deliver vaginally with careful planning, but critics say that patients must be given a full accounting of risks, including the possibility of fatal rupture. The coroner’s findings in Mabel Williams’s case emphasize the importance of transparent, evidence-based guidance and timely communication between maternity staff and expectant mothers.
As the families push for reforms, health officials face pressure to review both antenatal care protocols and the dissemination of information about birth options after cesarean. The coroner’s report suggests that improvements to leaflets and hospital policies could help ensure that future parents make informed decisions that reflect the most complete understanding of potential risks, including the possibility of a rupture that could endanger both mother and baby. In the meantime, Mabel Williams’s death remains a solemn reminder of the stakes involved in childbirth after cesarean and the need for vigilance in maternal health care.