Costa Café turned into makeshift ward at William Harvey Hospital amid NHS bed shortages
Campaigners condemn the move as humiliating as bed-blocking and corridor care strain East Kent hospitals and prompt calls for government funding
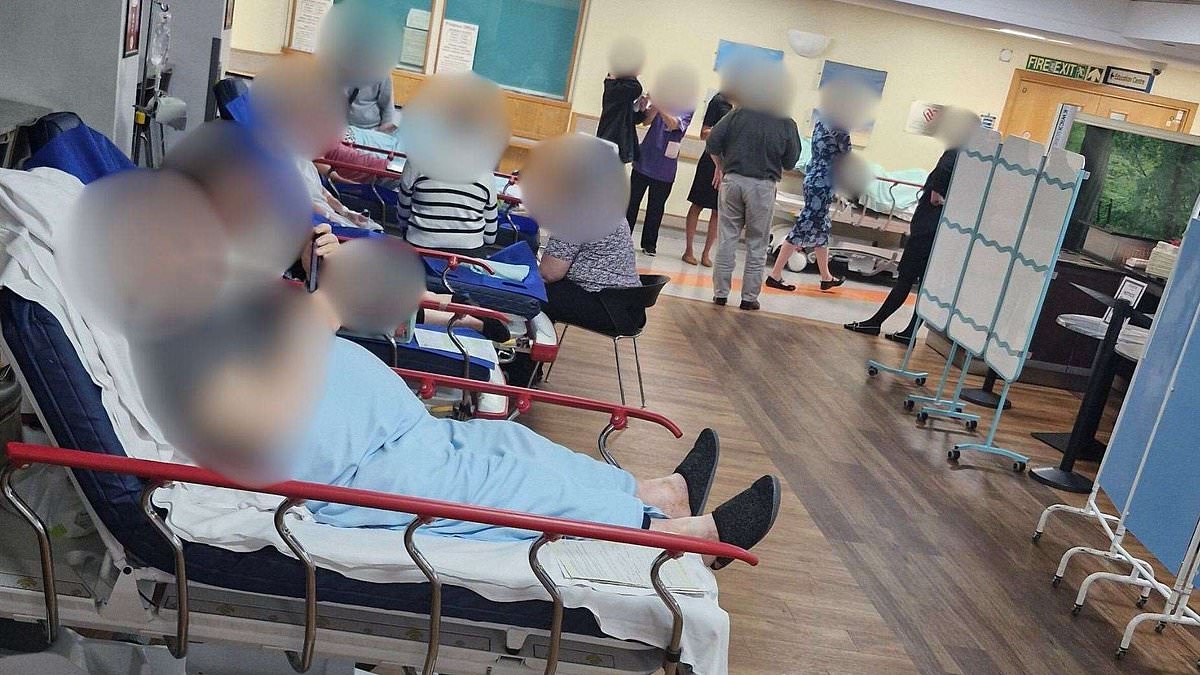
An overwhelmed hospital in Ashford has converted its Costa Café into a makeshift ward after space ran out on wards and in corridors, a situation health campaigners describe as humiliating for patients. The modification at William Harvey Hospital underscores the strain facing East Kent Hospitals NHS Foundation Trust and mirrors wider concerns about bed shortages, discharge planning, and the ability of hospitals to provide safe, dignified care.
Images circulating last week show elderly patients lying on beds wheeled into the Costa café area of the hospital, a scene that has prompted sharp criticism from relatives and campaign groups. A relative of a patient at the hospital said the arrangement reflects a broader squeeze on space and raised questions about whether patients are being treated with appropriate levels of dignity and oversight. Staff members have been overheard expressing frustration, with one colleague reportedly lamenting that Costa has been used again, while others stressed that there is simply no space left on wards or in corridors. The accounts point to a practice commonly described in the sector as bed-blocking, where patients ready for discharge remain in hospital because suitable care or placement is not available.
Ken Rogers, chair of Concern for Health in East Kent, called the makeshift ward horrendous and said it is absolutely disgusting for patients to be treated this way. He argued that shuffling patient beds into a nonclinical space due to a lack of ward capacity is horrific and highlights the urgent need for funding and systemic change to prevent a repeat. Rogers said he would press East Kent Hospitals to secure additional government support and plans to contact Health Secretary Wes Streeting to seek intervention as part of a broader push to address the crisis.
The predicament at William Harvey comes as East Kent Hospitals, which also runs the Queen Elizabeth The Queen Mother (QEQM) Hospital in Margate, has featured in national performance rankings. A government league table placed East Kent 101st among 134 acute care providers in a recent evaluation, illustrating persistent performance challenges. In August, 1,311 people waited at least 12 hours for a bed, up from 1,195 in the same month the previous year—the third highest level in England and a reflection of ongoing bed pressures across the region.
Bed-blocking and corridor care have become a focal point of criticism as hospitals struggle to admit, treat, and discharge patients efficiently. Sojan Joseph, the Ashford MP, labelled corridor care an unfortunate and unacceptable consequence of more than a decade of NHS funding pressures and cuts. He urged a pivot toward community-focused care, arguing that the government’s 10 Year Health Plan should accelerate moves away from hospital-centered care when safe and appropriate to do so. In Folkestone and Hythe, one of six pioneer sites in the government’s Neighbourhood Health Programme, planners aim to fuse medical and social care with local authorities and charities to create neighborhood teams capable of preventing hospital admissions and supporting long-term conditions before they escalate. Early pilots in the area reportedly reduced A&E attendances for at-risk patients from 223 to 33 within six months, a result officials say underlines the potential of closer, proactive care outside hospital walls.
The Neighbourhood Health Programme is supported by national funding of up to 10 million pounds, with the aim of easing pressure on hospitals by addressing problems earlier and closer to patients’ homes. NHS leaders hope the initiative will slow the slide toward episodic hospital care and reduce the need for makeshift solutions such as repurposing nonclinical spaces for patient care. The program’s rollout comes amid broader discussions about how to manage demand, improve discharge planning, and ensure that care pathways extend beyond hospital settings.
The controversy surrounding the Costa Café episode is echoed in the region by concerns about patient safety and dignity, as well as questions about the long-term viability of NHS capacity in Kent. Dorothy Reid, a 91-year-old patient who had previously waited hours for care after a back injury, sparked a formal inquiry when a North East Kent coroner ruled that the case highlighted a broader risk of future deaths if bed-blocking and lengthy A&E waits are not addressed. The coroner described the situation as a national crisis rather than a purely local one, underscoring the urgency of systemic reform to avert similar tragedies.
A spokesperson for the Department of Health and Social Care said the situation at William Harvey is unacceptable and that the hospital should take urgent action to address it. The department stressed that all NHS trusts must provide safe, dignified care in appropriate clinical settings and noted that the government inherited an emergency care system under significant strain. Officials added that winter-readiness measures, including war-game exercises and extra checks for vulnerable patients, are part of the strategy to ease hospital pressure and ensure timely access to care. East Kent Hospitals was contacted for comment as part of the inquiry into how to bolster capacity and improve patient experiences across the network.
The incident at William Harvey sits within a broader national conversation about hospital capacity, community care, and the evolving role of primary and social services in reducing demand on acute care. While the Neighbourhood Health Programme offers a potential pathway to relieve pressure in the region, advocates say it must be implemented consistently and funded adequately to produce lasting improvements. In the near term, campaigners, patients, and families will be watching closely to see whether the hospital system can avoid resorting to nonclinical spaces and maintain safety, dignity, and timely access to care for all patients.