Dense breasts can raise cancer risk up to six times; awareness and rising screening options push for personalized care
World Dense Breast Day highlights a condition affecting about half of U.S. women over 40, with calls for tailored screening and new research into blood-based tests.
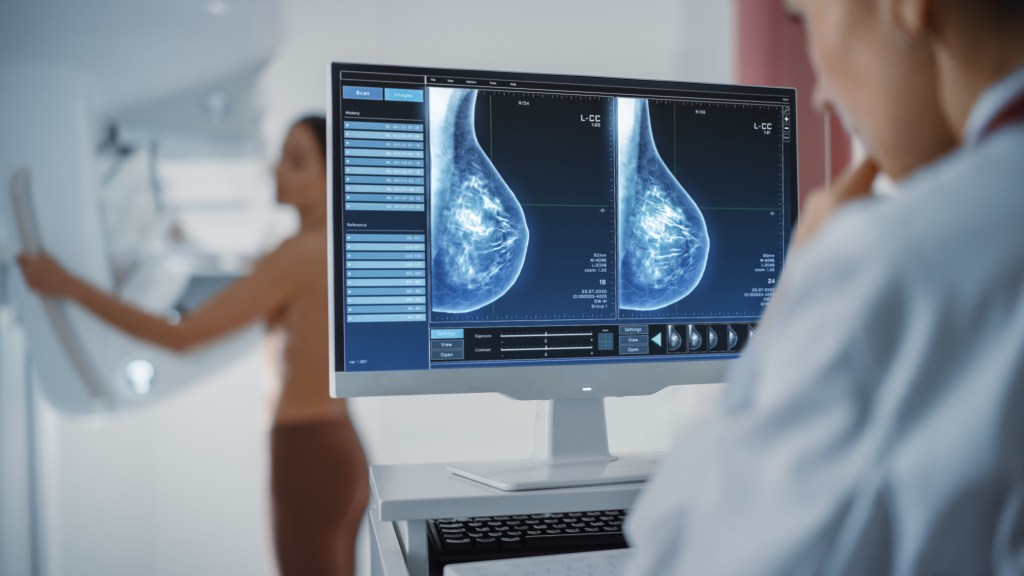
Dense breast tissue increases cancer risk and can obscure tumors on mammograms, doctors say, as World Dense Breast Day highlights a trait that affects roughly half of U.S. women over 40. Dr. Badri Konety, an oncologic surgeon and chief medical officer of Astrin Biosciences, described detection in dense tissue as “like trying to spot a snowball in a snowstorm.” The day underscores how density can both raise cancer risk and complicate detection, even as new testing approaches emerge.
Dense breasts are defined by the ratio of fibroglandular tissue to fatty tissue as seen on a mammogram. Fatty tissue appears dark on imaging, while fibroglandular tissue looks white. The more white tissue there is, the denser the breast. Density is about internal architecture, not how breasts feel. Smaller breasts can be extremely dense while larger breasts can be entirely fatty. Breasts are classified on the BI-RADS system from A to D: A is almost entirely fatty, B has scattered fibroglandular tissue, C is heterogeneously dense, and D is extremely dense.
Who’s more likely to have dense breasts? Genetics, race and age all play roles. Asian women, while typically having less breast tissue overall, have a higher percentage of that tissue being dense. Black women, on the other hand, tend to have more breast tissue overall but a lower percentage that is dense. Dense tissue is more common in younger women, and density can change over the life course, often declining after menopause.
Density matters because breast cancer is the most common cancer among American women and the second-deadliest, after lung cancer. In 2025, about 317,000 American women were expected to be diagnosed, with roughly 42,000 projected to die from the disease. Research shows women with extremely dense breast tissue are up to six times more likely to develop cancer than those with fattier breasts. Biologically, the fibroglandular tissue contains more cells that can become cancerous and harbors higher concentrations of growth factors and hormones that can promote tumor development. Dense tissue can also fuel inflammation and affect immune cells, creating conditions that may foster precancerous lesions.
Mammograms have long been the frontline screening tool, but their effectiveness wanes with density. Studies show mammograms can detect up to 98% of cancers in fatty breasts, but the detection rate can drop to as low as 30% in extremely dense tissue. The fundamental problem is visibility: both tumors and dense tissue appear white on mammograms, creating a “masking effect.” That can lead to interval cancers—tumors found between routine screenings that were likely present on a prior mammogram—occurring up to two to five times more often in women with dense breasts. Dense tissue can also complicate interpretation, increasing false positives.
You can’t tell whether your breasts are dense by feeling them. Density is about the internal architecture seen on imaging, not touch. In response to these limitations, the federal government now requires doctors to inform women about their breast density in mammogram result letters. Under the BI-RADS scheme, density is reported as either “dense” (categories C or D) or “not dense” (categories A or B). The notification also explains that density can hide cancers and may be linked to higher risk. Most guidelines recommend starting routine screening at age 40, and density information is typically available after the first mammogram.
What to do if you have dense breasts can depend on your overall risk. A full risk assessment, sometimes called CheckMate or a similar tool, can help determine next steps. Depending on the result, a clinician may discuss supplemental screening options such as ultrasound or an MRI. Insurance coverage for additional imaging varies and may not always apply to women without high-risk status, though many clinicians weigh benefits on a case-by-case basis.
There is new hope on the horizon. Companies like Astrin Biosciences are developing blood tests that could be reliable across all breast densities, including extremely dense tissue. The test analyzes more than 7,000 proteins in a single blood sample, searching for cancer signals that mammograms might miss. Early results are encouraging, with performance approaching MRI-level sensitivity in some studies. For the roughly 42 million American women with dense breasts who have long faced limitations of mammography, such a blood test could represent a potential game-changer when it comes to early cancer detection.
The test is not on the market yet, but experts advocate staying informed and proactive. Women should know their density, understand the implications, and engage in shared decision-making with their clinicians about screening options. If you’re uncomfortable with the limits of mammography in dense tissue, don’t wait for a yearly reminder—discuss your density, your risk, and your options with your doctor as part of a personalized screening plan.

In sum, World Dense Breast Day foregrounds a condition that affects many women and can both raise cancer risk and hinder early detection. As screening technology evolves, and as new blood-based approaches move toward market readiness, patients and providers alike are urged to integrate density into risk assessments and to tailor screening strategies accordingly. The overarching message is clear: knowledge of density empowers women to seek appropriate, timely care rather than accepting current screening limitations without question.