Doctors and surgeons warn as off-label use of Mounjaro and other weight-loss injectables spreads as an anti‑ageing shortcut
Clinicians say GLP‑1 and related drugs deliver metabolic benefits but are not proven ‘fountain of youth’; cosmetic specialists report rising demand for fillers to treat facial volume loss
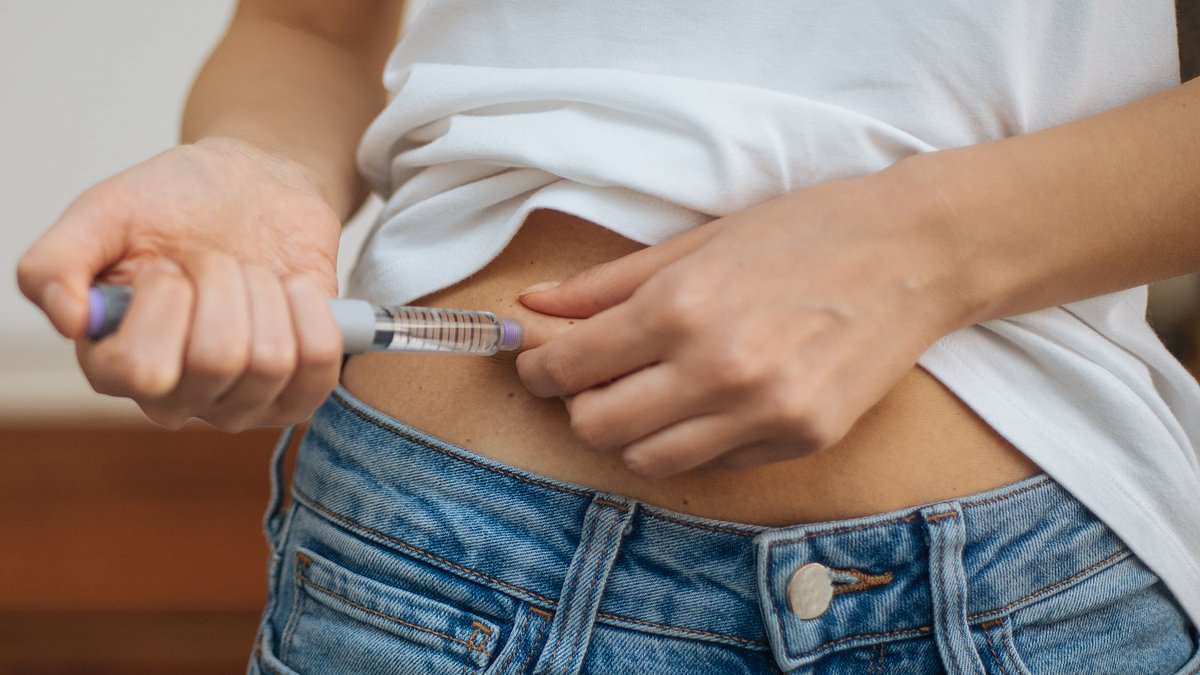
A surge in the use of injectable drugs such as Mounjaro, Ozempic and Wegovy for perceived anti‑ageing benefits has prompted concern from medical professionals and cosmetic surgeons, who say the medications can produce dramatic weight loss and metabolic improvements but are not proven to reverse cosmetic ageing and may carry side effects.
People who have adopted these medicines for off‑label cosmetic reasons and those who counsel patients say the trend is visible in some social circles, with private online groups trading tips about access and dosing and users reporting rapid facial thinning. Some cosmetic surgeons have seen a rise in requests for dermal fillers and other procedures to restore facial volume after patients begin treatment.
Manufacturers market the drugs for specific indications: semaglutide is sold as Ozempic and Wegovy and is approved for blood sugar control in type 2 diabetes and for weight management at higher doses; tirzepatide, marketed as Mounjaro, targets related metabolic pathways and is approved for diabetes with ongoing studies of its weight‑loss effects. These medications mimic gut hormones involved in appetite and glucose regulation, and clinical trials have shown reductions in weight, blood glucose and certain cardiovascular risk markers for some patients.
Despite these documented medical outcomes, clinicians caution against framing these medicines as an anti‑ageing solution. "There is no robust evidence that these drugs reverse the structural changes of skin ageing such as loss of collagen or elasticity," said a general practitioner who treats patients seeking metabolic therapy. Cosmetic specialists report that rapid reduction of subcutaneous fat in the face can create a hollowed appearance, which some patients then seek to correct with additional cosmetic procedures.
Anecdotal accounts circulated in social groups describe a range of experiences. Some users report dramatic weight loss and improvements in markers such as blood pressure and blood sugar. Others describe more troubling side effects, including sustained gastrointestinal symptoms, decreased energy, loss of muscle tone and mood changes. One person quoted in social commentary said they were hospitalised after severe gastrointestinal bleeding; that account has been reported as an individual claim rather than a verified medical finding in a broader dataset.
Clinicians emphasise that adverse effects are commonly gastrointestinal — nausea, diarrhoea, vomiting and constipation — and that more serious events, while less common, have been reported and require medical assessment. Physicians also warn that rapid calorie reduction and weight loss can lead to loss of muscle mass, changes in bone density over time and nutritional deficiencies if not supervised, particularly in people without clear medical need for the drugs.
The social dynamics surrounding the drugs are part of the current concern. In some communities, users have formed message groups named after active ingredients, and some prescribers report pressure to issue scripts for cosmetic reasons. Pharmacists and regulators in some jurisdictions have tightened scrutiny of prescriptions as demand has surged, and some clinics report prioritising patients with guideline‑based indications.
Public conversations have also turned to the appearance often called "Ozempic face," a colloquial term used to describe a gaunter facial appearance some people develop after losing facial fat. Cosmetic surgeons say they are seeing more patients seeking filler to restore mid‑face volume, jawline contouring or surgical options after weight loss induced by these medications. Those practitioners stress that any decision to combine metabolic drugs with aesthetic treatments should be undertaken with coordinated medical care.
Research into long‑term outcomes is ongoing. Randomised trials have demonstrated cardiovascular benefits for some patients on GLP‑1 receptor agonists, and scientists are examining whether metabolic changes might influence risks for conditions such as dementia. Investigators and regulators caution that such potential benefits do not equate to reversal of skin ageing or guaranteed improvements in appearance. Long‑term safety data, particularly for use outside approved indications or for populations without metabolic disease, remain limited.
Experts recommend that patients considering these medicines discuss them with a clinician, disclose their full medical history and be monitored for side effects, nutritional status and changes in muscle mass. They also urge realistic expectations: these drugs are indicated to treat metabolic disease and obesity in line with clinical guidelines, not as a cosmetic anti‑ageing panacea.
As the conversation about these medications continues, practitioners say responsible prescribing and clear patient education are essential. Regulators and professional bodies are watching trends in off‑label use and aesthetic demand, and clinicians encourage patients to weigh the known benefits and risks and to seek multidisciplinary care when aesthetic concerns arise after medical weight‑loss therapy.