Dry feet after pool visits: a personal health warning about athlete's foot and cellulitis
A London writer’s experience shows how neglecting moisture between the toes can spark a bacterial infection, with guidance on prevention and treatment from dermatology experts.
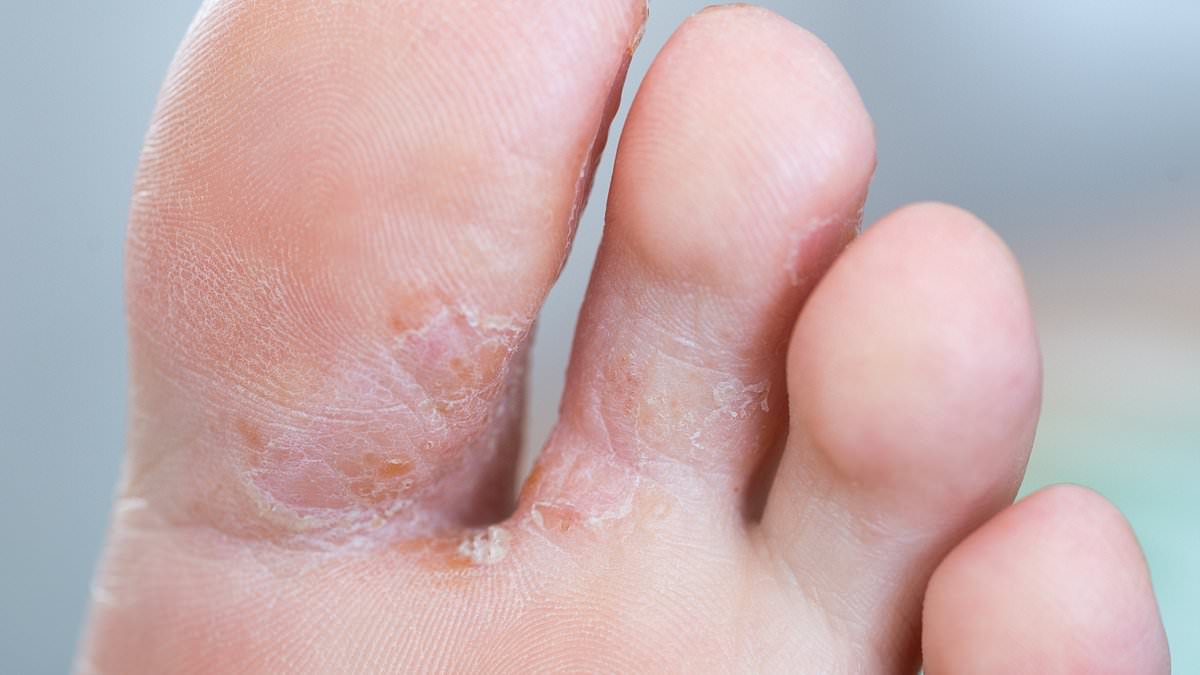
During a busy spell in central London, a freelance journalist describes how a routine lunchtime swim became a turning point in her health. In the rush to change after the pool, she skipped an essential step: drying the feet thoroughly, especially between the toes. What began as a familiar itch soon grew into something more serious, a warning about a common but often overlooked health hazard.
Over months she treated athlete’s foot with over‑the‑counter creams and powders, carrying a small pharmacy in her rucksack. The itching would ease, only to return. Then a strange numb burning sensation appeared at the front of the right foot, making every step feel off. On the train back to London she kept curling and uncurling her toes in her shoes. A comic limp followed, and after days she went to an emergency department. X‑rays were clear and she was told to elevate the leg and rest, but the heat and swelling continued to worsen. She would return to hospital multiple times, the doctors unsure what was going on, and a diagnosis eluding her until days later.
Two weeks of fluctuating symptoms and a growing concern culminated in a diagnosis that explained the pattern: a bacterial infection in the skin and the tissue underneath, called cellulitis. The explanation offered up a familiar mechanism: athlete’s foot can create cracks in the skin that allow bacteria such as Streptococcus or Staphylococcus aureus to enter. Once inside, the infection can cause skin that is hot, red, swollen and tender, and in some cases it can spread rapidly. The medical team started a course of antibiotics and cautioned that if there was no improvement, hospital admission might be required.
The treatment brought initial relief, but not a clean toll. After about seven days the heat and redness diminished, only to return with renewed intensity a few days later. The infection spread again up the leg, and walking remained painful. A GP offered a difficult diagnosis: the patient might be overreacting or anxious about the symptoms. A second course of antibiotics followed, and the writer reflects on the moment with a mix of humiliation and resolve. The entire episode—antibiotics and rest, hospital visits and fear—lasted roughly six weeks, during which every trip to the bathroom or step outside was a reminder of the fragility of the body's defenses.
Health professionals stress that while most cellulitis cases are mild to moderate and respond to antibiotics if caught early, the condition can spread quickly and, in the worst cases, lead to sepsis. Dermatology specialists outline how the initial fungal infection can set the stage for a bacterial one when the skin is damaged. The lesson is not simply about antibiotics, but about breaking a cycle of neglect and ensuring proper skin care and foot hygiene. They emphasize that the problem often begins with a simple crack in the skin from athlete’s foot, but it can also arise from other minor breaches such as insect bites or eczema. A practitioner notes that people should seek medical care promptly if the infection becomes red, hot, swollen, or if fever or malaise develops.
Prevention after an infection clears matters as well. Once athlete’s foot has resolved, it is important to keep feet dry, rotate shoes, and consider antifungal powder in shoes for those prone to sweating. Wearing footwear that breathes and avoiding damp communal changing areas can reduce risk. It is also wise to wipe all parts of the feet dry, including between the toes, and to be vigilant for any return of itching or redness. If redness or heat spreads, or if skin becomes painful or shows signs of swelling, seeking medical advice promptly is advised, particularly for patients with diabetes or compromised immune function.
The author concludes with a hard-worn lesson: the delay in doing the small, dull tasks—thoroughly drying the feet, finishing the antifungal course, and keeping footwear dry—came at the cost of weeks of treatment and a journey through the health system. Now, the approach to foot care is methodical: the antifungal course is finished in full, shoes are rotated to avoid moisture pockets, communal showers are navigated with flip‑flops, and any early sign of redness or warmth is treated seriously. The experience underscores a broader message for public health: common infections can escalate quickly if not addressed, and careful daily hygiene remains a simple, effective line of defense.