Drying feet after public swims linked to cellulitis: a cautionary health tale
A journalist’s experience underscores the importance of thoroughly drying between toes to prevent serious skin infections.
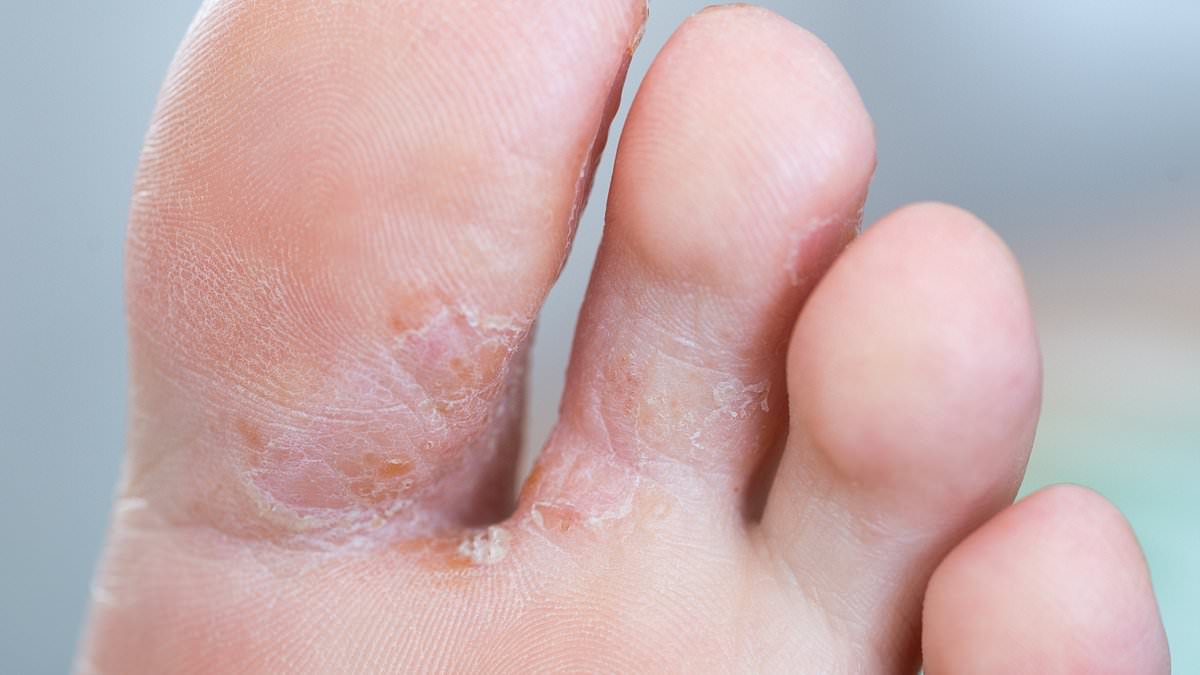
A routine attachment to lunchtime swims near central London turned into a serious health scare after a simple, often overlooked habit was neglected: drying the feet, especially between the toes. A journalist recounts how rushing to get back to the desk after a 40-minute session at a tucked-away Soho pool contributed to a bacterial skin infection that required antibiotics and, at one point, hospital treatment. The episode highlights how a common foot condition can escalate when basic hygiene steps are skipped.
The author describes the weekly pattern that kept stress in check amid a fast-paced work life. The swims occurred at Marshall Street Leisure Centre, a small, quiet space where the city noise seemed to fall away. Drying off and getting dressed quickly became part of a hurried routine. In the rush to move on with the day, the crucial step of drying between the toes was often skipped. He had a familiar pharmacy toolkit—antifungal creams and powders—to manage athlete’s foot, a common fungal infection that thrives in warm, damp skin, especially when toes aren’t thoroughly dried. He would shake a tube of Canesten into his rucksack one month, then Lamisil the next, hoping to keep the condition under control. He knew the routine well because previous bouts of athlete’s foot had taught him that moisture and warmth create a fertile ground for fungal growth.
The trouble did not appear immediately. The itch would come and go, a nuisance that could be managed with over‑the‑counter remedies. But over time the symptoms changed character. While pursuing an MA at the National Film and Television School in Beaconsfield and freelancing as a journalist, the author began to notice a numb, burning sensation at the front of his right foot, a sensation that made every step feel wrong. It felt as if the ground itself had tilted. He would coil and uncoil his toes in his shoes during seminars and train rides, hoping the odd feeling would pass. He did not yet know that the combination of damp feet and a cracked barrier in the skin could invite bacteria to invade deeper tissues.
The diagnosis would come only after days of escalating symptoms and a trek through A&E that left him waiting for hours. At first he suspected a broken toe, but the real problem lay beneath the surface. The first week or so produced only a comic limp and mounting concern from his tutors and friends who watched the hobble worsen. The nurse-like waiting rooms and quiet hallways were punctuated by the heat and swelling creeping up the leg. The first set of X‑rays showed nothing obvious, but the persistent redness and tenderness could not be ignored. The author describes it as a turning point that forced a reckoning with a condition he had often treated as a minor nuisance.
Eventually the clinical picture clarified: a bacterial infection in the skin and the tissue beneath, known as cellulitis. The doctors explained that the most common culprits are Streptococcus and Staphylococcus aureus, bacteria that live harmlessly on the skin but can enter through cracks—such as those caused by athlete’s foot—and trigger a deeper infection. The explanation underscored a stubborn truth: simple skin breaks can be a gateway for more serious problems if not treated promptly. As the infection spread, the author experienced increasing heat, redness, and tenderness in the affected area, with the edge of the rash climbing higher up the leg. The medical team emphasized that cellulitis can progress quickly and, if untreated, may lead to sepsis in the worst cases, though most instances are mild to moderate and resolve with antibiotics when caught early.
After an initial course of antibiotics, the improvement appeared dramatic at first. The relief was short-lived; a week later, the redness returned, the swelling grew, and every step sent a jolt of pain through the calf. A GP visit confirmed the seriousness of the situation, and the possibility of needing further hospital treatment loomed. The clinician’s tone was cautious, and a moment of self‑doubt followed before a second course of antibiotics was prescribed. The author reflects on a moment when a colleague’s casual observation, then a whispered label—neurotic—felt like a sting to the ego in the face of a real medical concern. It was a sobering reminder that health, not perception, must guide action.
Overall, the episode lasted about six weeks from the initial warning signs to full recovery. In that time, simple daily acts—bathroom trips, showers, and even stepping into shoes—were transformed into careful, sometimes painful rituals. The author’s experience underscores several key lessons echoed by dermatologists and general practitioners: athlete’s foot is common and usually manageable at home, but cracks in the skin can let bacteria in and lead to cellulitis; early recognition and treatment are critical; and prevention hinges on dry feet, clean and breathable footwear, and prompt response to new or spreading symptoms.
Dermatologists emphasize a three-step approach for dealing with athlete’s foot. Step One is to begin using an over-the-counter antifungal cream at the first sign of infection, with continued use for two to six weeks and for one to two weeks after symptoms clear to prevent relapse. Step Two advises seeing a GP if symptoms do not improve with self-care or if the area feels hot and painful, with a higher index of concern for people with diabetes or a weakened immune system. Step Three focuses on prevention after clearing an infection: regular washing and thorough drying of feet, wearing breathable socks, and keeping footwear dry, including applying antifungal powder in especially prone cases. These steps, supported by comments from Dr Leila Asfour, a dermatologist and spokesman for the British Association of Dermatologists, and Professor Kamila Hawthorne, chair of the Royal College of General Practitioners, align with the author’s own experience: neglecting to dry between the toes and delaying treatment can transform a mild fungal issue into a bacterial infection that demands antibiotics and, in rare cases, hospitalization.
The health episode also served as a caution about changing-room environments, where damp floors and shared facilities can be a convergence point for both fungal and bacterial infections. The doctors stressed that red flags—redness that spreads, warmth, swelling, new blistering or fever—should prompt urgent medical attention. They also noted that while athlete’s foot can trigger cellulitis, it is not the sole cause; a blister, insect bite, or eczema patch can open the same door for bacteria entering through compromised skin.
In the end, the author embraced a more deliberate routine: completing the full antifungal course, rotating shoes to avoid dampness, wearing flip-flops in communal showers, and acting quickly if redness or heat returns. The takeaway is clear: the time saved by rushing through routine foot care can be costly in the end. The six-week recovery reinforced a simple truth for health: dull, repetitive care—drying between toes, drying thoroughly after any moisture exposure, and responding to early signs of infection—can prevent the kind of escalation that disrupts daily life and threatens well-being.