Full‑body MRI flags early fatty liver and gallstone in 25‑year‑old wellness reporter
A consumer MRI service identified liver enlargement and a gallstone linked to insulin resistance; physicians weigh benefits and risks of direct‑to‑consumer whole‑body scans.

A full‑body MRI purchased from a consumer imaging service detected a slightly enlarged liver and a gallstone in a 25‑year‑old health reporter, findings that physicians say can be signs of early nonalcoholic fatty liver disease and insulin resistance.
The scan, performed by Ezra — a direct‑to‑consumer imaging company owned by Function Health — did not identify any urgent abnormalities, but five days after the exam a doctor‑reviewed report noted sinus inflammation, small ovarian cysts and the liver changes. The company advertises a 22‑minute basic MRI covering 13 organs for $499 and says its scans have helped 6% of members catch potential cancer early.
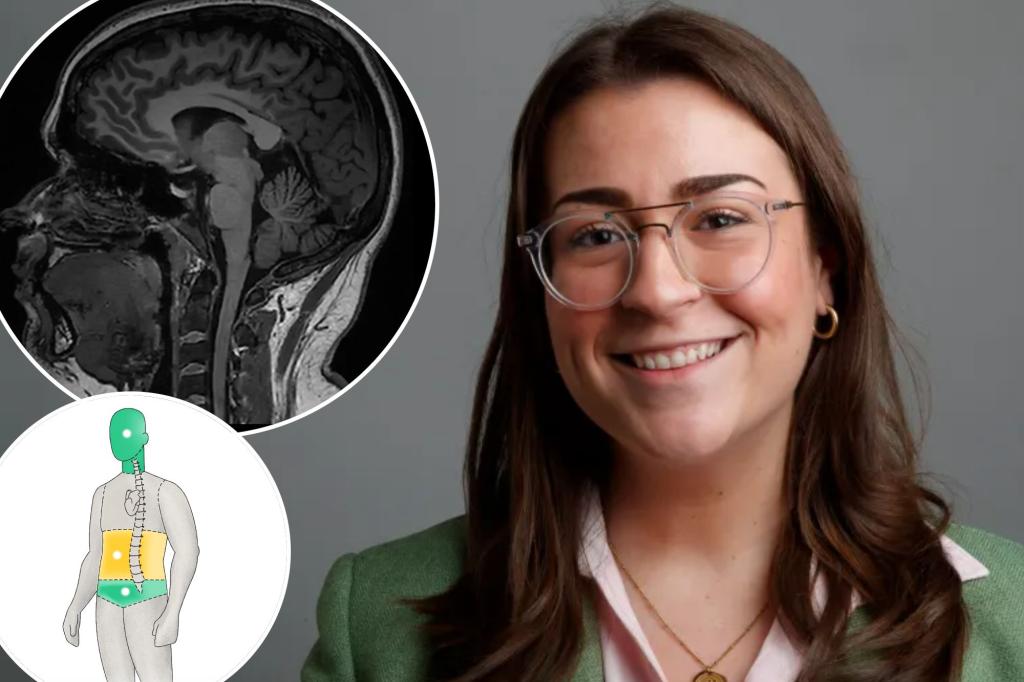
The reporter described the exam as brief and noninvasive: changing into provided attire, wearing earplugs and lying in the MRI while coils captured images of the brain, liver, kidneys and other organs. The experience took less than an hour from arrival to completion. Magnetic resonance imaging uses magnetic fields and radio waves to create detailed images of internal organs and soft tissues.
A physician who reviewed the reporter’s scans, Dr. Mark Hyman, said the combination of a mildly enlarged liver and a gallstone, together with prior blood tests showing slightly elevated fasting insulin, was consistent with early fatty liver and insulin resistance. Hyman, a co‑founder of Function Health, advised dietary changes, reducing acetaminophen use, and considering supplements such as N‑acetyl cysteine and alpha‑lipoic acid to improve liver function and metabolic markers.
Proponents of consumer whole‑body imaging argue that broader access to advanced scans can catch conditions before they cause symptoms, potentially improving outcomes. Ezra and other companies have received celebrity endorsements and market the scans as a preventive tool. But some physicians caution that screening low‑risk people can produce incidental findings that trigger anxiety, follow‑up testing and invasive interventions that may not be necessary.
Nonalcoholic fatty liver disease, or NAFLD, occurs when excess fat accumulates in the liver and can progress to inflammation, fibrosis and cirrhosis. It is closely linked to metabolic dysfunction and insulin resistance. Hyman described NAFLD as a "silent epidemic" and said it affects a large portion of the U.S. population; physicians and public‑health agencies have reported rising prevalence as obesity rates climb. NAFLD often produces few or no early symptoms, and when present they can be nonspecific, including fatigue and abdominal discomfort.
Critics of direct‑to‑consumer full‑body scans say three issues merit attention: the potential for false positives or incidentalomas, out‑of‑pocket costs for scans and follow‑up care, and the clinical value of detecting subclinical findings in otherwise low‑risk individuals. Medical societies generally recommend targeted imaging based on symptoms or risk factors rather than routine whole‑body screening for asymptomatic people.
Supporters say that, when paired with clinical interpretation and appropriate follow‑up, imaging can reveal treatable conditions earlier. Ezra’s basic package is intended to flag abnormalities across organs including the brain, liver and kidneys, and its reports include plain‑language explanations and suggested next steps. The company operates multiple centers in New York City and has expanded to other locations, and its marketing has featured public figures who said the scans were worthwhile.
The reporter’s scan prompted practical next steps recommended by the reviewing physician: lifestyle changes to address insulin resistance, including reducing refined carbohydrates and sugars; scaling back regular use of acetaminophen; and medical follow‑up to monitor liver tests and metabolic markers. Hyman also said supplements might help some patients but that clinical decisions should be individualized.
Experts emphasize that not every abnormality on an MRI represents immediate danger, and many findings resolve or remain stable without invasive treatment. They recommend that consumers considering direct‑to‑consumer imaging discuss the decision with a primary care clinician, understand the limits of screening, and be prepared for potential downstream testing.
The reporter, who sought the scan in part because of a family history of diabetes, heart disease and Alzheimer’s, reported feeling relieved that the exam found no urgent conditions and said the results helped identify a manageable metabolic issue earlier than routine care might have. Dr. Hyman characterized the findings as useful for early intervention: "You're a classic example of someone who’s walking around at 25, thinking you’re healthy and invincible — but you have things that, one, affect how you feel now, and two, significantly raise your risk going forward," he said.
Public‑health experts note that the broader challenge is addressing metabolic dysfunction at the population level through proven measures such as diet, physical activity, screening for diabetes and cholesterol management. For individuals, imaging can be one tool among many for identifying risk, but clinicians stress that imaging results should be interpreted in the context of clinical history, laboratory data and established guidelines.
The debate over the role of consumer full‑body MRIs is likely to continue as companies expand offerings and patients seek more information about their health. In the meantime, clinicians say attention to diet, physical activity and routine preventive care remains the cornerstone of reducing the risk of conditions associated with fatty liver and insulin resistance.