High blood pressure at age 7 linked to greater midlife cardiovascular death; experts urge childhood screening
Analysis of 38,000 US children followed for five decades found elevated childhood blood pressure associated with up to a 50% higher risk of cardiovascular death, prompting calls for routine checks amid differing national policies.
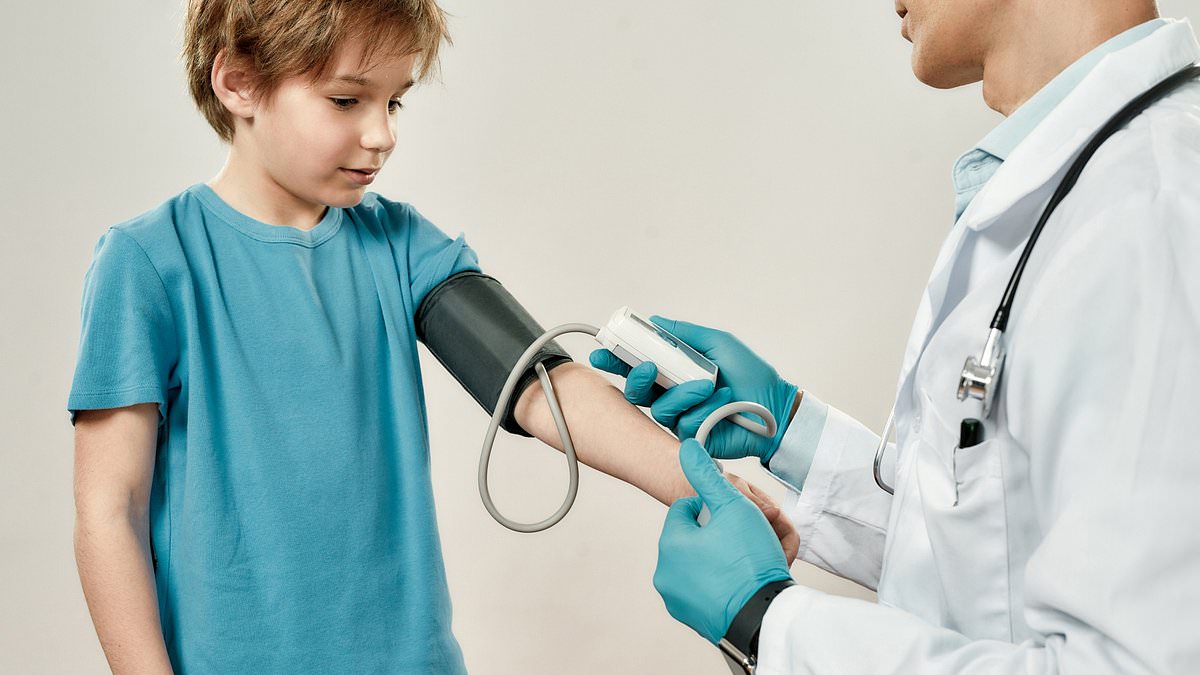
A new long-term study found that children with higher blood pressure at age 7 faced a substantially increased risk of dying from cardiovascular disease by middle age, and researchers are calling for routine blood pressure screening in childhood to help prevent fatal heart disease decades later.
The team analysed data on about 38,000 children whose blood pressure was measured at age 7 as part of a longstanding US cohort and followed their health for an average of 54 years. Children whose blood pressure measurements were in the highest decile for their age, sex and height had the greatest excess risk, with researchers reporting an approximately 40–50% higher likelihood of cardiovascular death over the ensuing five decades compared with peers with lower readings.
Alexa Freedman, lead author and researcher at Northwestern University in Chicago, said the findings were unexpected in their magnitude and persistence. "Specifically, having hypertension or elevated blood pressure as a child may increase the risk of death by 40 per cent to 50 per cent over the next five decades of an individual's life," Freedman said in a statement accompanying the study. The results were published in JAMA and presented at the American Heart Association Hypertension Scientific Sessions 2025 in Baltimore.
The research team said the results underscore the potential value of identifying elevated blood pressure in childhood so that clinicians, parents and public health systems can promote cardiovascular health from an early age. They noted that earlier detection could support efforts to establish heart-healthy habits, monitor trends, and intervene when appropriate.
Clinical practice in the United States differs from the United Kingdom. The American Academy of Pediatrics recommends that blood pressure be measured at annual paediatric appointments starting at age 3. In the UK, routine blood pressure screening for children is not currently recommended. The UK National Screening Committee has cited uncertainties about how many children have hypertension, the long-term impact, the availability of an accurate screening test for young people, and how best to prevent progression to adult disease.
Commenting on the new findings, Bonita Falkner, emeritus professor of paediatrics and medicine at Thomas Jefferson University, said the study supports monitoring blood pressure as an important marker of cardiovascular health in childhood. Other earlier studies have similarly linked elevated blood pressure in older children and adolescents with higher risks of cardiovascular events in adulthood.
High blood pressure, or hypertension, often has no obvious symptoms but increases the risk of heart attacks, strokes and other organ damage if left untreated. Blood pressure is recorded as two numbers: systolic pressure (the higher number, when the heart pumps) and diastolic pressure (the lower number, the resistance in blood vessels). As general adult guidelines, readings of 140/90 mmHg or higher are often considered high, while readings between 120/80 mmHg and 140/90 mmHg may indicate increased risk.
Public health officials and clinicians note that high blood pressure is far more common in adults than children, and that research into childhood hypertension faces challenges including changing normal ranges with growth, the need for age- and height-adjusted thresholds, and variability in measurement techniques. The UK screening committee has also cautioned that it is not yet clear how screening children at scale would alter long-term outcomes.
The study adds to a body of evidence suggesting that cardiovascular risk factors measured in childhood can have lasting consequences. The researchers called for greater attention to routine measurement and follow-up in paediatric care, while acknowledging that any policy changes would need to consider test accuracy, resource implications and evidence on effective early interventions to reduce long-term risk.
Health authorities, paediatricians and policymakers will need to weigh the new findings alongside existing recommendations and practical considerations, including how best to measure blood pressure in young children, how to confirm elevated readings, and what lifestyle or medical interventions are safe and effective when initiated in childhood. The study provides long-term observational evidence linking childhood blood pressure and midlife cardiovascular mortality but does not by itself establish which screening or treatment strategies will optimally reduce that risk.