High-fat, ultra-processed diet alters memory cells in days, UNC study finds
Mice given a Western-style high-fat diet showed hyperactivity in hippocampal CCK interneurons and impaired memory within four days; intermittent fasting and restoring glucose reversed the effect.

Researchers at the University of North Carolina School of Medicine report that eating an ultra-processed, high-fat diet can disrupt how the brain forms new memories within days, well before obesity develops.
In a study published last week in the journal Neuron, investigators found that mice fed a diet modeled on the Western pattern — rich in cheeseburgers, fries and ice cream-style foods — developed abnormal activity in a specific set of hippocampal neurons called cholecystokinin-expressing (CCK) interneurons after just four days. The hyperactivity impaired the animals’ ability to process new memories, the team said.
"We knew that diet and metabolism could affect brain health, but we didn’t expect to find such a specific and vulnerable group of brain cells, CCK interneurons in the hippocampus, that were directly disrupted by short-term high-fat diet exposure," said Juan Song, the study’s principal investigator and a professor of pharmacology at UNC. "What surprised us most was how quickly these cells changed their activity in response to reduced glucose availability, and how this shift alone was enough to impair memory."
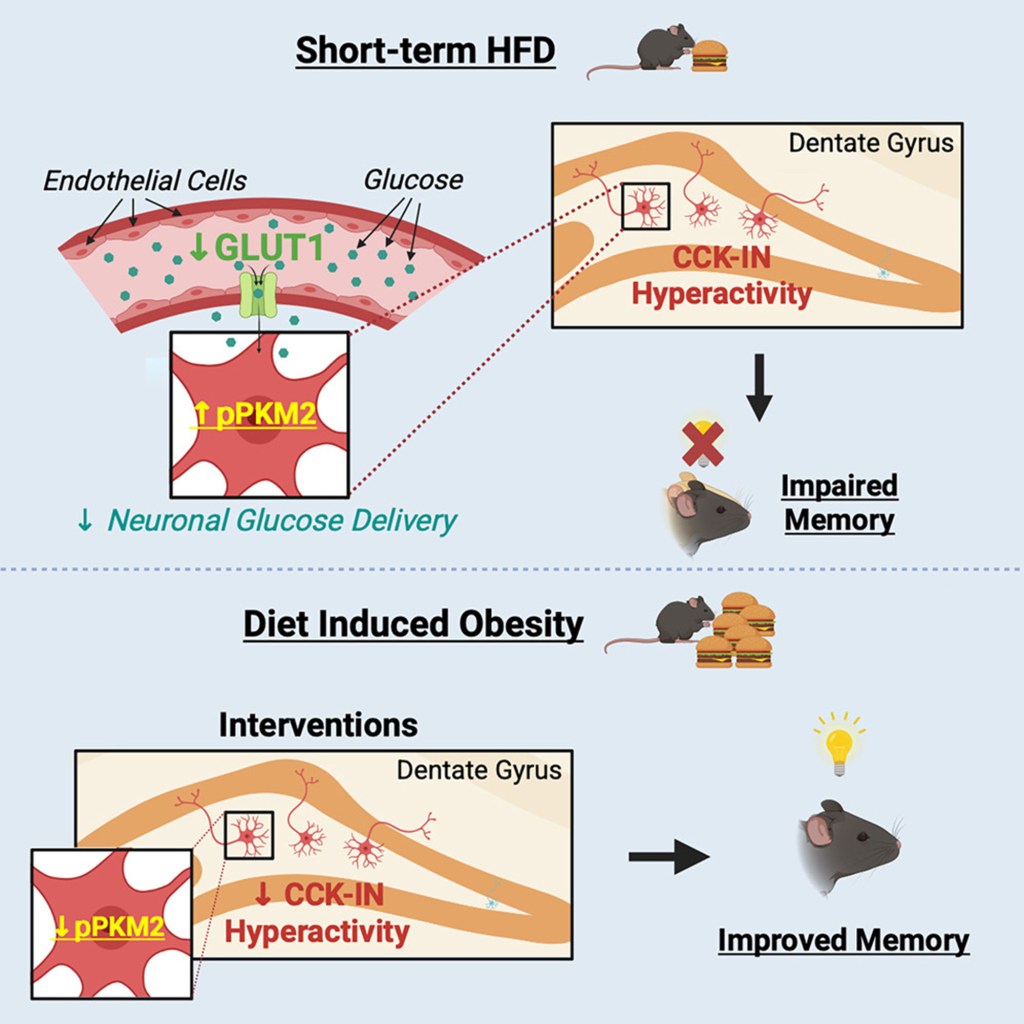
The researchers report that consumption of the high-fat diet interfered with the brain’s sugar metabolism and reduced glucose availability. That metabolic shift was associated with increased firing of CCK interneurons, which in turn disrupted hippocampal circuits responsible for encoding new experiences.

The changes occurred on a timescale too short to be explained by weight gain or obesity-related damage. Obesity is a chronic, progressive condition known to affect brain health through reduced blood flow, loss of brain volume and inflammation, but the UNC team emphasized that the new findings show damage can begin before those long-term processes are evident.
The study tested whether correcting glucose availability or altering metabolic signaling could reverse the effect. Intermittent fasting — defined in the study as a regular period without calories — normalized CCK interneuron activity and improved memory performance in the mice. Restoring glucose availability also returned interneuron activity toward baseline levels.
Researchers identified pyruvate kinase M2 (PKM2), an enzyme that helps regulate the final step of converting sugar to energy, as a key molecular player. Reducing the activity or expression of PKM2 mitigated the interneuron hyperactivity in the experimental animals. The paper notes that existing drugs and interventions, including the diabetes drug metformin, the immunomodulatory agent rapamycin, certain herbal compounds and calorie restriction, have been shown in other studies to affect PKM2 activity.
Song and colleagues caution that the experiments were performed in mice and that translating findings to humans requires further work. Still, they said the rapid onset of neural and behavioral changes underscores the sensitivity of hippocampal circuits to short-term dietary and metabolic shifts.
The study adds to a body of research linking diet quality to cognitive function. Previous human and animal studies have associated diets high in antioxidants, healthy fats, fruits, vegetables, whole grains, nuts and seeds with better brain structure, function and memory. Conversely, regular consumption of ultra-processed, high-fat foods has been associated with impaired memory and an increased risk of neurodegenerative conditions such as dementia and Alzheimer’s disease.
Dementia is characterized by progressive loss of memory, reasoning, judgment and language skills and is not considered a normal part of aging. The UNC team said it will continue to investigate whether the mechanisms they identified contribute to the development of Alzheimer’s disease and whether diets that support brain glucose regulation can offer protective benefits.
The findings suggest potential interventions that could be tested in humans, from dietary approaches that maintain brain glucose availability to pharmacologic targeting of metabolic enzymes such as PKM2. The researchers stressed that their immediate next steps include further preclinical work to map the molecular pathways and to evaluate longer-term consequences of intermittent exposure to high-fat diets.
Health professionals not involved in the study said it reinforces existing public health guidance emphasizing a diet rich in whole foods and limited in ultra-processed items, particularly for populations at risk of cognitive decline. The study’s authors noted that simple changes in eating patterns may have rapid effects on brain function and that both dietary and metabolic therapies warrant further clinical investigation.