Measles-related brain disorder kills Los Angeles child, highlighting SSPE risk years after infection
Health officials warn about subacute sclerosing panencephalitis, a rare, nearly always fatal complication that can arise years after measles. The case comes as vaccination rates dip in parts of the United States.
LOS ANGELES — A school-age child in Los Angeles County has died after developing subacute sclerosing panencephalitis, a rare but deadly brain disorder that can surface years after a measles infection. Health officials said the child contracted measles as an infant, before receiving the measles, mumps and rubella (MMR) vaccine, which is typically given in two doses starting at 12 to 15 months. The case is the latest reminder of measles’ long-tail risks and comes as measles-related deaths are being tracked by federal health authorities.
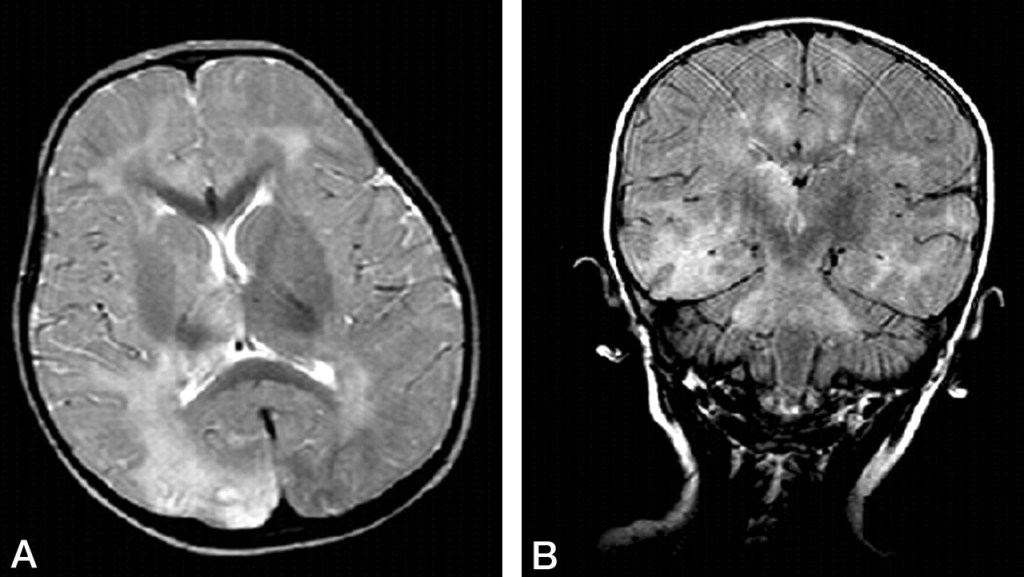
Subacute sclerosing panencephalitis (SSPE) occurs when the measles virus persists in the body and gradually mutates. It typically begins with mood changes or behavioral shifts, followed by cognitive decline, seizures and motor problems, and progresses to severe brain damage and death. The progression usually unfolds six to 10 years after the original infection. Medical literature estimates that four to 11 of every 100,000 measles cases develop SSPE, and the disease carries a mortality rate around 95 percent with no known cure. Brain imaging has shown characteristic patterns in SSPE, underscoring the condition’s devastating impact on neural tissue.
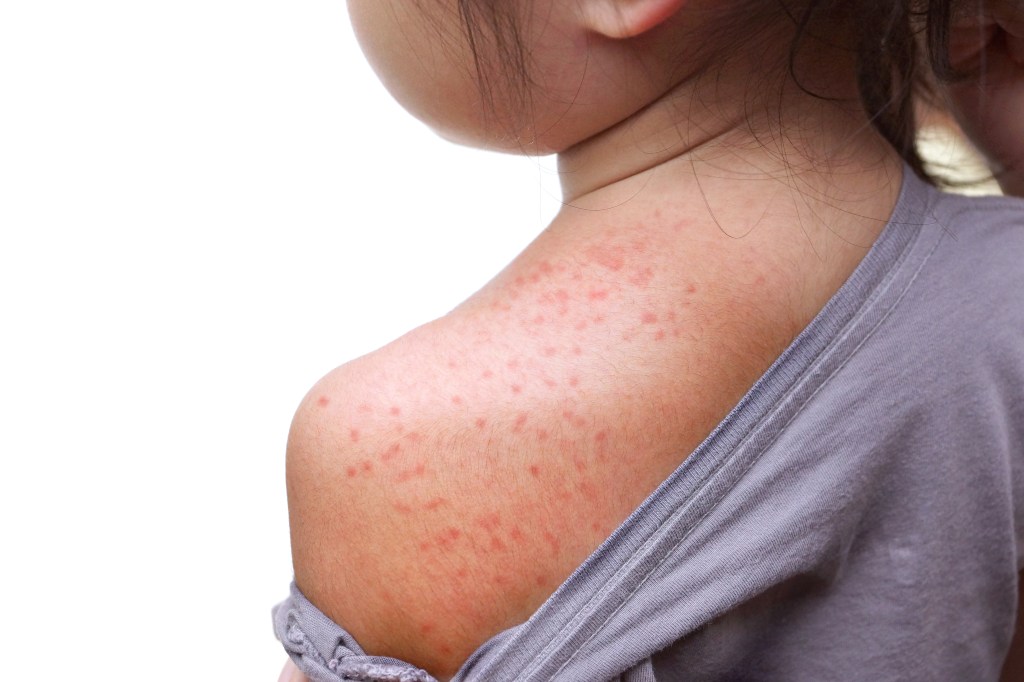
Measles is a highly contagious respiratory illness that spreads easily through droplets in the air. Pneumonia is the most common complication, but the infection can also lead to bronchitis, laryngitis and, in very rare cases like the California case, SSPE years after the initial illness. The risk of long-term brain damage underscores why health officials emphasize vaccination as a critical public health tool.
Vaccination remains the best protection against measles and its complications. The MMR vaccine is about 97 percent effective and has prevented millions of deaths globally since it was introduced. The first dose is routinely administered at 12 to 15 months, with a second dose given before kindergarten or first grade to ensure more complete protection. Infants and toddlers who are too young to be vaccinated rely on community immunity—high vaccination coverage among those around them—to reduce exposure risk and transmission. Despite this, immunization rates for MMR and other routine childhood vaccines have declined in the United States since the COVID-19 pandemic.
A recent analysis found that 92.5 percent of kindergarteners were vaccinated against MMR for the 2024-25 school year, down from 95 percent in the 2019-20 school year. Experts attribute part of the decline to lingering misinformation about vaccines, including fraudulent claims that the MMR vaccine is linked to autism—a theory that has been debunked repeatedly by scientists. “Declining vaccination rates stem partly from fraudulent research attempting to link the MMR vaccine to autism,” Benedict Michael, a professor of infectious neuroscience at the University of Liverpool, wrote this week in The Conversation. “Social media misinformation has amplified these fears, potentially worsened by COVID pandemic skepticism around vaccines.” The MMR vaccine’s efficacy and the broad protection it offers remain central to public health messaging as measles cases rise in parts of the country.
From the CDC: 1,491 measles cases have been reported so far this year as of this week. About 92 percent of patients were unvaccinated or had unknown vaccination status, and 12 percent of cases required hospitalization. Most of the hospitalized patients are children under five. “The death in L.A. serves as an important reminder that measles is not a benign childhood illness,” said Benedict Michael’s colleague, who emphasized the need for widespread vaccination to shield vulnerable populations. “It can cause serious complications, including pneumonia and, as this case shows, delayed but deadly brain damage years later.”
The Los Angeles County health official overseeing child health emphasized that protecting infants who cannot yet be vaccinated depends on broad community immunity. “Infants too young to be vaccinated rely on all of us to help protect them through community immunity,” said Dr. Muntu Davis in a statement released last week. “Vaccination is not just about protecting yourself — it’s about protecting your family, your neighbors and especially children who are too young to be vaccinated.”
Public health officials continue to urge vaccination for measles and other routine childhood diseases as a core strategy to reduce preventable illnesses and prevent rare, long-term complications like SSPE. The Los Angeles case, while singular, adds to a growing concern that rising measles exposure in communities with lower vaccination rates could yield more severe outcomes years down the line.