Melbourne trend: GLP‑1 weight‑loss injections promoted as anti‑ageing, sparking concerns
A Daily Mail columnist describes widespread use of Mounjaro, Ozempic and similar drugs among suburban women chasing youth, prompting reports of gaunt faces, side effects and more cosmetic procedures.
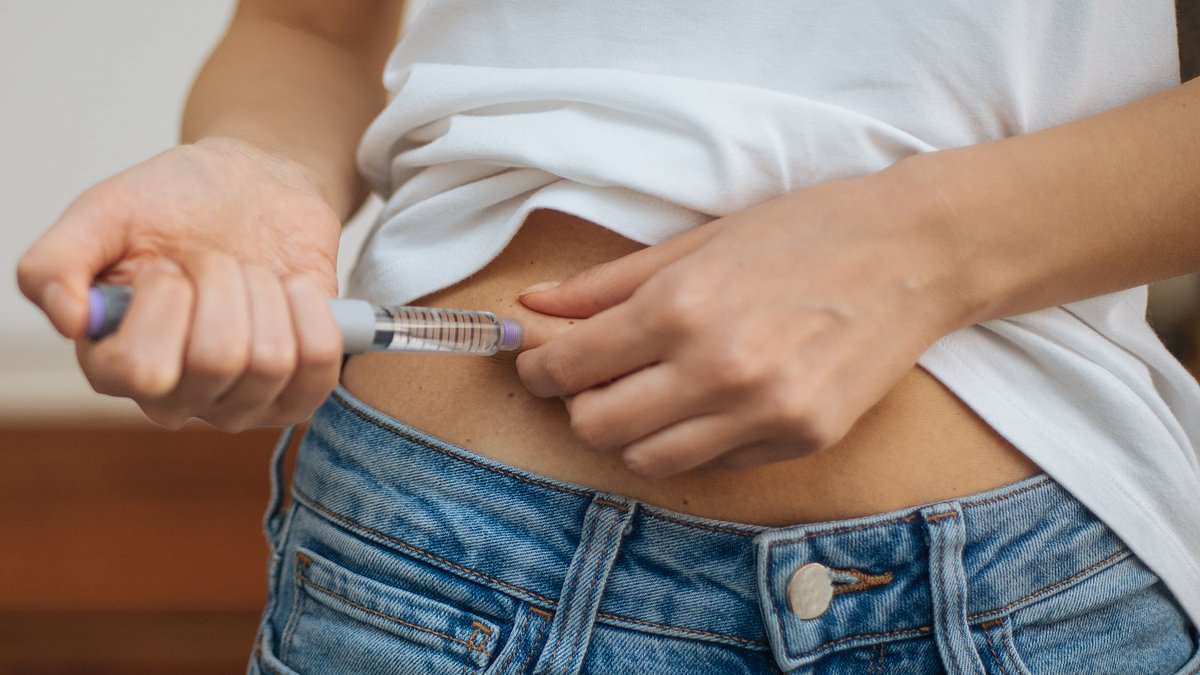
Women in parts of Melbourne have embraced injectable GLP‑1 medications such as Mounjaro and Ozempic not only for weight loss but increasingly as a purported route to “looking younger,” a trend that has prompted concern from some users and cosmetic practitioners.
In a column published in the Daily Mail, writer Amanda Goff described seeing the drugs used widely in affluent Melbourne suburbs, with women discussing semaglutide‑based treatments in WhatsApp groups and at social gatherings. Goff wrote that while the medications deliver dramatic weight loss and measurable health benefits, many users report unintended cosmetic and health consequences, including a hollowed facial appearance and adverse gastrointestinal symptoms.
Goff wrote that some women she knows have stopped treatment after experiencing loss of muscle definition, persistent low energy and depressed mood. She also relayed an anecdote in which a friend said she experienced rectal bleeding and required hospital care after starting an injection. Those accounts were presented as personal reports collected by the columnist.
The drugs involved — marketed under brand names including Mounjaro (tirzepatide), Ozempic and Wegovy (both containing semaglutide) — belong to a class called GLP‑1 receptor agonists. They mimic a hormone that regulates blood sugar, suppresses appetite and can reduce inflammation; studies and prescribing information note benefits such as weight loss and improvements in blood pressure and metabolic markers, and some research suggests reduced risks for cardiovascular events and possibly dementia.
Medical and cosmetic practitioners have reported a rise in patients seeking facial filler and other treatments to address a gaunter look after rapid weight loss, a phenomenon sometimes described in media coverage as “Ozempic face.” Cosmetic surgeons told the Daily Mail they have seen increased demand for procedures to restore facial volume as more people use these medications.
Experts emphasise that weight loss — whether achieved through medication, diet or surgery — can reduce facial fat and alter contours, and that those changes are not direct signs that a drug does or does not have broader anti‑ageing effects. The column quoted cosmetic practitioners observing requests to correct facial hollowing and sagging that patients associate with the injections.
The Daily Mail piece also described social drivers in some Melbourne suburbs, saying that treatment use has spread through social networks and local culture, with Goff contrasting the local trend with the lifestyle of women in Sydney’s Bondi area, who she described as relying more on exercise and other non‑pharmacologic beauty measures.
Public discussion about GLP‑1 drugs has broadened since their expansion into mainstream obesity treatment. Regulators approve several GLP‑1 receptor agonists for type 2 diabetes and for weight management in people with obesity or overweight and related health conditions; clinicians increasingly prescribe them off label or for cosmetic weight loss, which has fuelled demand and media attention.
Clinicians and public‑health experts have warned that using prescription medications for cosmetic or off‑label purposes carries risks that should be weighed against potential benefits. Reported side effects of GLP‑1 medications include nausea, vomiting, diarrhoea and less common but serious events; individual experiences vary widely. The accounts in the Daily Mail column were anecdotal and reflect the observations of one writer and her acquaintances.
As use of these medications becomes more visible in social settings, some users and clinicians say more patient education is needed about expected outcomes, possible adverse effects and the ways rapid weight loss can change facial appearance. Others emphasise the documented clinical benefits for people with metabolic disease and significant obesity and recommend that prescribing and monitoring remain in the hands of qualified clinicians.
The trend described in the column highlights a broader public‑health conversation about demand for pharmacologic shortcuts to cosmetic goals, the role of social influence in medical decision‑making, and how clinicians should balance benefits and harms as GLP‑1 drugs reach a wider consumer market.