Northwestern Medicine opens longevity clinic in Chicago, linking aging pace to Amish genetics
The clinic offers a four-hour, $4,200 protocol measuring multiple health metrics to inform lifestyle choices, grounded in research on PAI-1 and Amish genetic mutations.

CHICAGO — Northwestern Medicine’s Human Longevity Clinic opened in July in the heart of Chicago, offering a four-hour, $4,200 protocol designed to gauge how a person’s body ages and to arm patients with information that may motivate lifestyle changes. The clinic, led by medical director Dr. Baljash Cheema, conducts a comprehensive battery of tests intended to map an individual’s aging pace rather than diagnose a disease today.
The itinerary covers a wide swath of physiology, including imaging, blood work, cognitive tasks and physical challenges. In the author’s experience, the process began with body composition analysis via a dual-energy X-ray absorptiometry (DEXA) scan, which takes about seven minutes. A phlebotomist drew six vials of blood to assess metabolic balance, while the clinical team prepared for technologically driven assessments that go beyond routine annual checkups. The tests continued with spirometry, where the patient blows into a mouthpiece while wearing a nose clip to gauge lung function, and a series of cognitive tasks that include word recall and a clock-drawing exercise. The day ends with sensory and motor evaluations, including eye photography, hearing tests and an assessment of olfactory function with smells such as strawberry and leather. [IMAGE: ]
There are 14 major components in the protocol, and many tests are performed in a single session to create a detailed health profile. Cheema said the goal is to map where a patient stands relative to their peers and to highlight modifiable factors that could influence aging trajectories. “We’re a clinic for people that are curious about these health metrics and want to know more,” Cheema said. “The intent is to get a sense of where you’re at and to arm you with information that may motivate you to make change.” He cautioned that the clinic does not prescribe interventions that lack solid scientific backing, stating, “We will not recommend people to do things … that are not rooted in science.”
The clinic’s approach traces to research around a protein called PAI-1, which helps regulate blood clotting but also appears to influence aging across several organ systems. Northwestern’s work on PAI-1 grew from studies by Dr. Douglas Vaughan, director of the Potocsnak Longevity Institute at Northwestern’s Feinberg School of Medicine. Vaughan observed that some members of a Swiss Amish community in Indiana carry a genetic mutation that results in very low PAI-1 levels and, as a result, longer, healthier lives. He and colleagues developed testing protocols that measure aging rate in those individuals, which Cheema said the clinic has translated into a clinical program while acknowledging that many questions remain unanswered. The project sits within an ecosystem of science and global partnerships meant to ground clinical practice in evidence.
The testing protocol includes body composition analysis, cardiovascular and respiratory assessments, neurological screening, sensory evaluations, and mobility testing. The author’s experience featured several elements deemed routine in longevity-focused programs, but the breadth was striking. The DEXA scan, described above, was complemented by bloodwork that evaluated metabolic markers; the cardio-respiratory test suite included VO2 peak estimation during treadmill activity, with the patient wearing a mask that recorded respiratory data as speed and incline increased. The clinic’s leaders describe this as an opportunity for patients to see how their bodies respond to stressors and to translate that information into practical changes. [IMAGE:  ]
]
The clinical visit also encompassed sensory and motor evaluations intended to flag early signs of cognitive decline. In the author’s case, the results highlighted a balance challenge: the sharpened Romberg test, which measures steadiness with one foot in front of the other, showed a notably short duration with eyes closed. Cheema acknowledged that many people struggle with balance and noted that these results aren’t uncommon among a population of midlife adults discovering their health baselines. Hearing tests revealed an asymmetry: the left ear did not register the highest frequency tested, near 4,000 hertz, which is adjacent to the upper range of a typical piano keyboard. The eye and nose assessments were less dramatic, but the measurements contributed to a holistic portrait of health that went beyond a single number.
The most striking takeaway for the author was the range reported by multiple aging clocks, which used AI-based and molecular timing methods to estimate cellular age. The clocks produced a span from 34 to 44 years old — a reminder that aging is a mosaic of different biological processes that can diverge from an individual’s calendar age. Cheema emphasized that hormones and other internal factors can influence these clocks, particularly for individuals who have undergone fertility treatments or other medical interventions. The goal, he said, is to “arm you with information that may motivate you to make change,” rather than to present a definitive verdict on life expectancy.
Following the assessment, Cheema offered a set of personalized recommendations grounded in science and tailored to the patient’s results. The plan included augmenting endurance training with higher-intensity interval training to improve cardio-respiratory fitness and incorporating strength training to build muscle and reduce fat. Cheema cautioned that recommendations should be implemented with caution and under proper supervision, noting that the clinic does not promote unproven supplements or nutraceuticals. He suggested ongoing monitoring and a mid-year check-in to gauge whether the suggested changes moved the needle on the patient’s metrics. The author’s follow-up was scheduled for six months after the initial visit to repeat blood work and assess progress toward the stated targets. The broader aim, Cheema said, is to encourage patients to adopt sustainable changes that could influence aging trajectories over time.
The clinic is already attracting a diverse crowd. Cheema said patients range from people in their 20s to those with chronic conditions who want a clearer sense of where they stand. He said the results have generally been “not earth-shattering” but still meaningful, offering a granular look at the patient’s health status. A recurring theme is the discrepancy between perceived and actual health metrics: many patients underestimated their body fat percentage or overestimated their peak cardiovascular fitness. The clinic’s approach is to present data in a way that helps patients set realistic, scientifically grounded goals.
In the broader health landscape, Northwestern’s longevity clinic is one of several hundred such facilities worldwide — with estimates suggesting as many as 800 longevity centers in the United States alone. The field blends clinical care with research, sometimes moving into areas that require careful interpretation. Cheema stressed that the clinic’s protocol builds on Northwestern’s research partnerships across the globe and aims to contribute to a growing body of knowledge about aging and health. The clinic’s leadership contends that the focus should stay on scientifically validated practices and that any recommendations be grounded in evidence rather than speculation. The emphasis on ongoing research and yearly follow-ups signals an intent to treat aging as a dynamic process rather than a one-off test result.
Beyond Northwestern, the broader public interest in longevity has drawn attention from technology-focused figures who pursue intensive, daily aging testing. The piece references Bryan Johnson, a tech entrepreneur known for his extreme personal aging program, as a point of comparison for the level of testing some individuals pursue. The authors acknowledge that Johnson’s approach is far more time-intensive than what a typical patient would undertake in a clinical setting, highlighting the spectrum of choices available for people who want to understand and potentially influence their aging processes.
For patients, the clinic presents a structured, science-based pathway to understand health metrics that often change gradually. It does not aim to diagnose disease in its current form, but it seeks to identify early signs of risk and to offer actionable steps that may alter future health outcomes. Cheema underscored the responsibility of clinicians to avoid overinterpretation and to ensure that recommendations are anchored in robust science. He also stressed the value of longitudinal data: yearly visits and regular blood work can reveal trends that single-point readings cannot, helping to refine lifestyle prescriptions over time.
As the aging-health landscape continues to evolve, Northwestern’s longevity clinic offers a window into a future where individuals can proactively map their biological aging and, if needed, adjust daily habits with professional guidance. The emphasis remains on evidence-based practice, patient education and ongoing research. Whether such clinics become a mainstay of routine care or remain a niche pursuit will depend on continued scientific validation, accessibility and the willingness of patients to invest time, money and effort into long-term health monitoring. In the meantime, patients like the author leave with a clearer sense of where they stand and concrete steps designed to help them move toward healthier aging. [IMAGE: 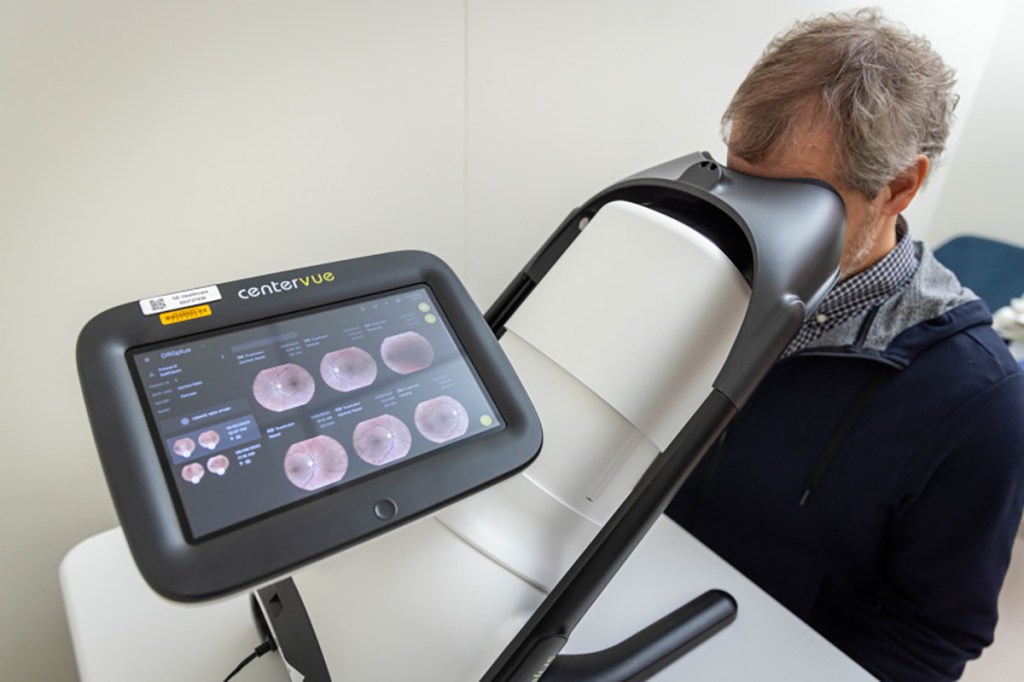 ]
]
As aging science advances, the Northwestern program and its peers will likely expand the menu of tests and refine the way results are translated into day-to-day behaviors. The underlying principle remains consistent: even modest improvements in fitness, diet, sleep and cognitive health can accumulate over years, potentially altering how gracefully a person ages. For now, patients can pursue a structured, medically supervised look at their aging process and use the insights to shape a healthier path forward, one test, one workout, and one well-informed decision at a time. [IMAGE:  ]
]
The clinic’s existence underscores a broader shift in health care toward proactive, data-driven personalization. Whether patients choose to participate in this model depends on their goals, resources and comfort with the pace of interpretation. But for those who want to understand how aging manifests in real-time—and what can be done to influence it—the Northwestern program offers a detailed, clinician-guided platform to begin that journey.