Scotland’s largest health board pays £3.6m to set up 1,000‑bed ‘virtual hospital’
NHS Greater Glasgow and Clyde signs three‑year deal with London firm Doccla to remotely monitor patients as services grapple with extensive waiting‑time backlogs
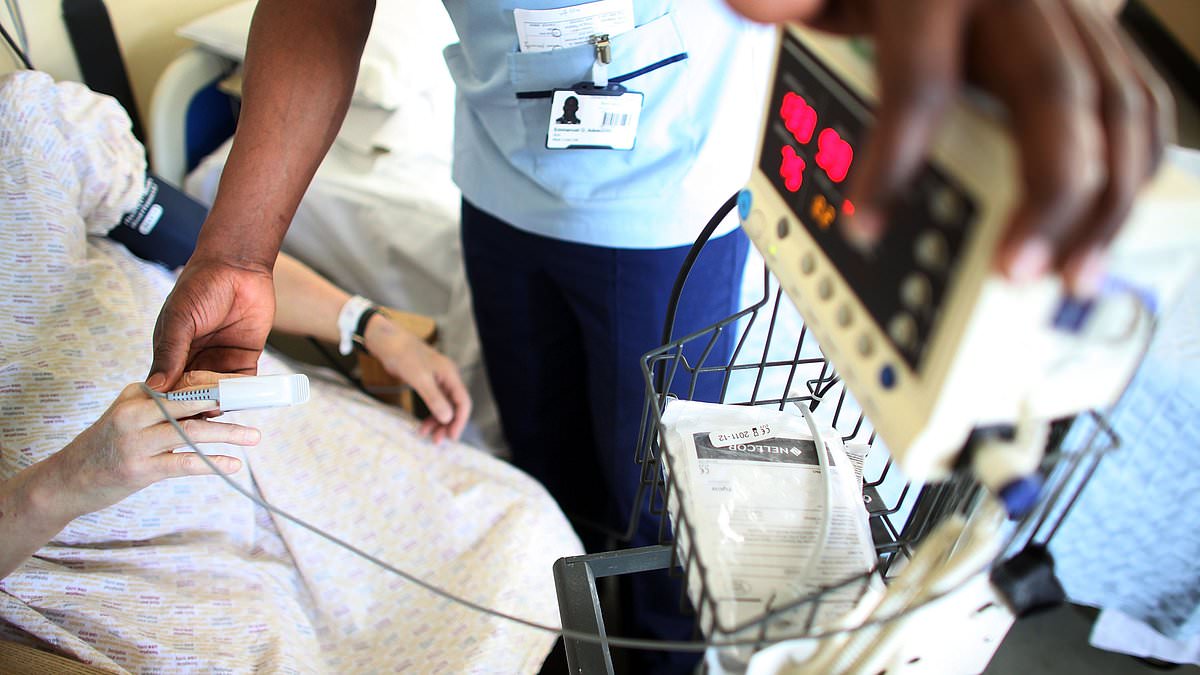
NHS Greater Glasgow and Clyde (NHSGGC) has agreed a £3.626 million, three‑year contract with London‑based medical technology firm Doccla to create a 1,000‑bed “virtual hospital” that will monitor patients at home, the health board said on Saturday.
Under the arrangement, NHSGGC will issue devices that record blood pressure, temperature, heart rate, activity levels and oxygen saturation and link the readings to a smartphone app. The system will also enable video calls and messaging between patients and clinical teams, with the stated aim of reducing hospital admissions, shortening inpatient stays and increasing capacity for in‑person care.
NHSGGC described the service as a digital remote monitoring system that will support 1,000 virtual beds and clinics, and said the virtual hospital “will play a significant role in the transformation of services.” Documents disclosed to the press show the total set‑up cost as £3,626,777.
The move comes as Scotland’s health services face sustained pressure from long waiting lists and missed performance targets. The Daily Mail reported that NHS Scotland is consistently missing the four‑hour target for emergency departments; the paper cited statistics showing that in July, of 140,820 people attending emergency departments, 71.1% were seen, admitted, transferred or discharged within four hours, below the 90% target. In a single week ending Aug. 31, NHSGGC recorded 2,277 patients who waited more than four hours for emergency care.
Scottish politicians and clinicians have offered mixed responses to the announcement. Scottish Conservative health spokesman Dr. Sandesh Gulhane said frontline staff were “overworked and under‑resourced” and described remote monitoring as a “sticking plaster” that would not replace in‑person care. Scottish Labour health spokeswoman Jackie Baillie pointed to more than 880,000 people she said are on waiting lists and warned that long backlogs were driving some patients to seek private treatment.
Scottish Labour analysis cited in media coverage compared long‑term waits in Scotland with those in England, reporting nearly 15,000 people in Scotland waiting two years or more for treatment versus 182 in NHS England. The analysis said long waits are far more common in Scotland on both absolute and population‑adjusted bases.
Health Secretary Neil Gray has previously signalled that a Scottish Government pledge to ensure no one waits more than a year for NHS treatment by March 2026 may be abandoned, a development cited by critics as evidence of increased pressure on services.
NHSGGC said the virtual hospital model is designed to provide clinicians with continuous, remote patient data so that decisions about admission, discharge and ongoing care can be made more quickly and safely. The health board said the contract is for a digital remote monitoring system that will support virtual beds and clinics and that the programme could cover up to 1,000 patients at a time.
Clinical leaders and health officials have been piloting remote monitoring and virtual ward approaches across the UK as part of efforts to manage demand and reduce avoidable hospital stays. Supporters argue such systems can free beds and focus in‑person resources on the most acutely ill, while critics caution they risk shifting responsibility to patients and do not address staffing shortages that drive delays in care.
NHSGGC did not give a specific start date for the service in its statement but said the contract was agreed for three years. The health board said it will monitor the programme’s effect on admissions, length of stay and capacity as the service is rolled out.