Shorter 15‑minute prostate MRI matches standard scan in trial, could expand screening access
International PRIME trial finds a two‑part, non‑contrast MRI detects clinically important prostate cancer at the same rate as the current three‑part scan while halving time and cost
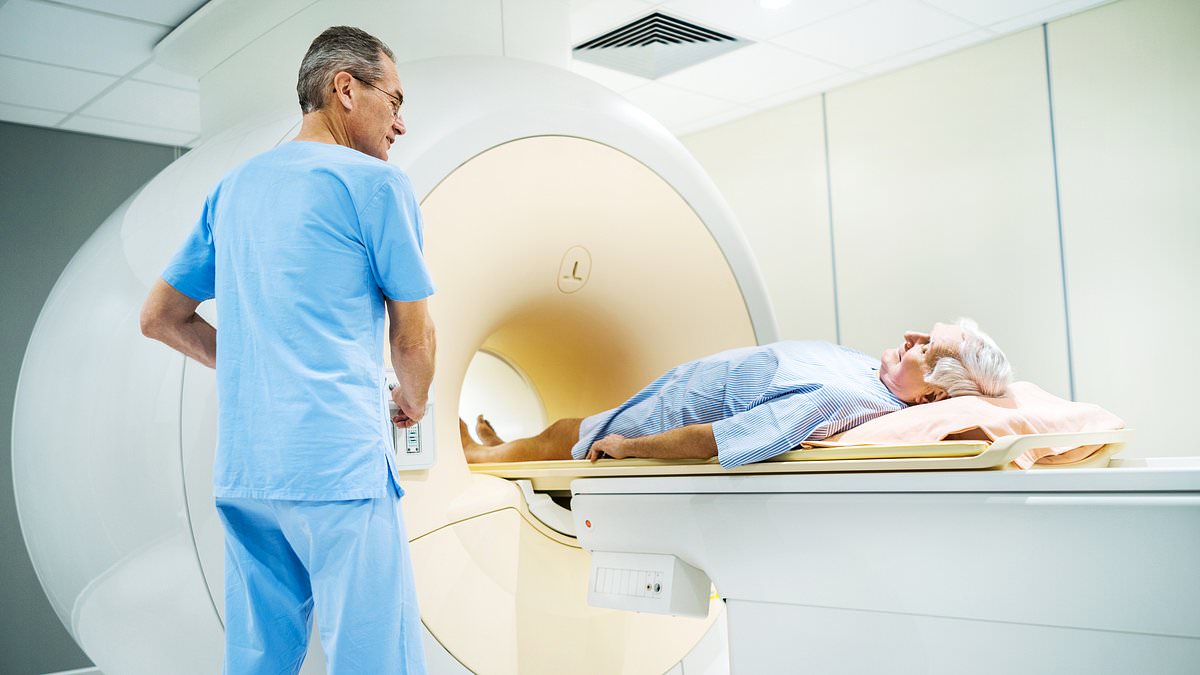
A streamlined 15‑ to 20‑minute prostate MRI detected clinically important cancer at the same rate as the standard 30‑ to 40‑minute scan in a landmark international trial, researchers reported, a finding they say could increase access to imaging and support moves toward a national screening programme.
The PRIME trial enrolled 555 men aged 59 to 70 across 22 hospitals in 12 countries to compare a two‑part “biparametric” MRI that omits contrast dye with the conventional three‑part “multiparametric” MRI that includes a contrast stage. All participants underwent the full three‑part scan; radiologists reviewed images from the two‑part protocol without knowledge of the contrast results and separately reviewed the full scan. Prostate biopsy was used when indicated to confirm diagnoses. The shorter scan identified clinically important prostate cancer in 29% of patients, the same proportion detected by the full scan.
Researchers reported the two‑part protocol takes roughly half the time of the standard scan, requires fewer staff, and is 47% cheaper. On the NHS, a three‑part scan costs an average of about £273, and the contrast stage typically requires the presence of a clinician. The PRIME trial was funded by the John Black Charitable Foundation and Prostate Cancer UK and the findings were published in JAMA.
"Currently around four million MRI scans are needed each year globally to diagnose prostate cancer," said Associate Professor Veeru Kasivisvanathan, chief investigator of the trial and a researcher at UCL Surgery & Interventional Science and UCLH. "Time, cost and staff availability are all limiting factors in how many scans can be offered, which makes the results of the PRIME trial particularly important. If we can do the scan in up to half the time, with fewer staff and at lower cost, that will make a huge difference in allowing every man who needs a scan to be able to get one in a timely fashion."
Lead radiologist Associate Professor Francesco Giganti, also of UCL and UCLH, said the contrast injection used in the three‑part MRI can rarely cause mild side effects and requires additional time and clinician involvement. He warned that shorter protocols must be of high diagnostic quality and interpreted by radiologists with dedicated expertise in prostate MRI.
Magnetic resonance imaging has markedly changed prostate cancer diagnosis over the last decade by enabling targeted biopsies and allowing men with normal scans—around a third of patients—to avoid unnecessary biopsy. Despite the benefits, only 62% of men who needed a prostate MRI in England and Wales received one in 2019, the most recent year for which data are available.
Prostate cancer is the most common cancer in men in the UK, with about 56,000 diagnoses and roughly 12,000 deaths annually. The NHS currently runs national screening programmes for breast, bowel and cervical cancers but not for prostate cancer. The UK National Screening Committee is reviewing recent developments in prostate cancer diagnosis and is due to report later this year.
The trial’s findings have been cited as relevant to ongoing policy discussions. Health Secretary Wes Streeting has expressed support for a national prostate cancer screening programme, indicating sympathy for proposals to initially target high‑risk groups. Former prime minister Rishi Sunak and other politicians have also backed calls for targeted screening.
Separately, Prostate Cancer UK is due to begin the Transform trial later this year, described as the largest prostate cancer screening trial in two decades, which aims to identify the most effective screening approach and provide evidence for any future national programme. Dr Matthew Hobbs, director of research at Prostate Cancer UK, said the PRIME results are an important step toward making MRI more efficient and that the combined evidence from the two trials should inform guideline reviews.
Researchers and advocates cautioned that any change in practice should preserve diagnostic quality. They urged that scans be performed and interpreted to high standards and that national guideline bodies, including NICE and the National Screening Committee, consider the accumulating evidence when deciding on screening policy and practice changes.
The PRIME findings suggest a faster, cheaper MRI protocol could allow more men timely access to imaging and reduce barriers posed by scanner time, staffing and cost, while additional large‑scale screening trials and guideline reviews progress.