States Move to Expand Access to COVID-19 Vaccines After FDA Limits
Governors, health departments and pharmacy boards issue standing orders and executive directives to broaden eligibility and let pharmacists vaccinate, citing professional society guidance
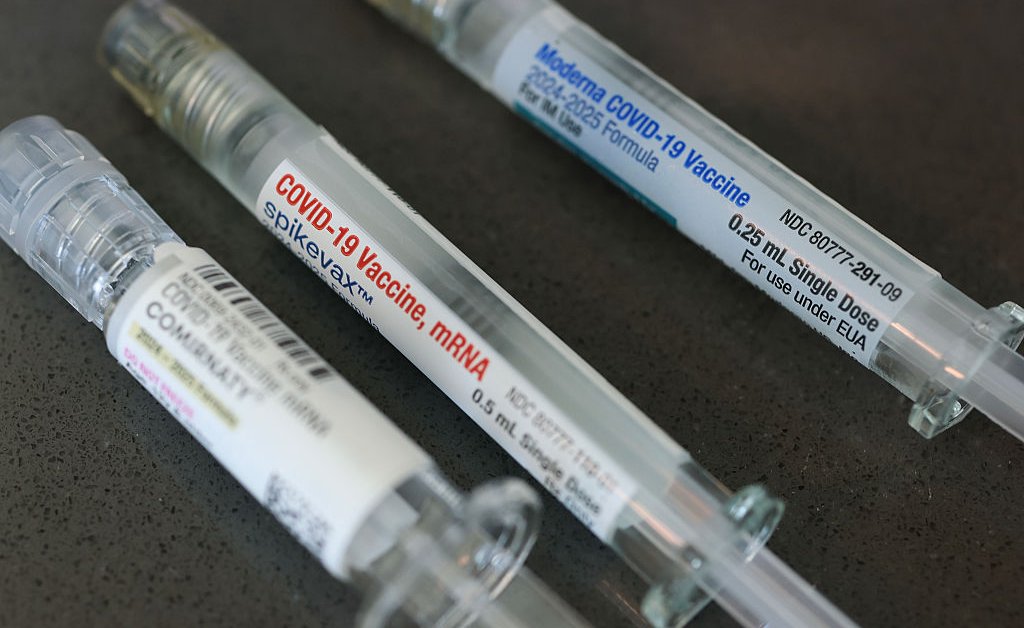
States across the United States have moved to preserve or broaden access to COVID-19 vaccines after the Food and Drug Administration last month authorized updated shots with eligibility limited to people 65 and older and those with underlying health conditions. The federal decision marked a major change from earlier policy and, according to reporting, ran counter to recommendations from some FDA scientists, prompting a patchwork of state-level responses to ensure wider access.
Since the FDA announcement, a number of professional medical groups have issued guidance that diverges from the federal authorization. The American Academy of Pediatrics recommends the vaccine for children ages 6 to 23 months, and the American College of Obstetricians and Gynecologists recommends vaccination for pregnant and breastfeeding people. Several states cited such recommendations or their own immunization advisory bodies when issuing orders and guidance to expand who can receive the shots and who may administer them.
Arizona Gov. Katie Hobbs on Sept. 12 signed an executive order directing the state Department of Health Services and Board of Pharmacy to make the recently approved COVID-19 vaccine, along with other vaccines, broadly accessible. “Vaccines are critical tools that safeguard public health and prevent serious illness,” Hobbs said in a release announcing the order, which the governor said would allow Arizonans and their doctors to access the vaccine if it is right for them.
Colorado’s public health order, issued by the Colorado Department of Public Health and Environment, permits pharmacists to provide the COVID-19 vaccine to anyone 6 months or older beginning Sept. 5. The order, announced by Gov. Jared Polis, is effective until Sept. 4, 2026, unless altered or rescinded. Polis said the move was intended to make it easier for Coloradans to get the updated COVID vaccine and flu shots this fall without having to see a doctor first.
Connecticut officials coordinated across departments to encourage continued vaccination access despite federal changes. The Connecticut Department of Public Health released guidance informed by the American Academy of Pediatrics and encouraged pharmacists to keep administering shots. The state insurance regulator also said COVID-19 shots must be covered by state insurance policies regardless of federal Advisory Committee on Immunization Practices recommendations.
Illinois Gov. J.B. Pritzker signed an executive order on Sept. 12 creating a "Statewide Vaccine Access Initiative." The order directs the Illinois Department of Public Health to work with state agencies and community partners to publish plain-language guidance, support school-based vaccination efforts, and issue a standing order allowing providers to administer vaccines recommended by the state’s Immunization Advisory Committee. The committee was scheduled to meet Sept. 22, and the department was directed to issue public guidance by Sept. 26.
Minnesota Gov. Tim Walz issued an executive order on Sept. 8 directing the Minnesota Department of Health to identify and remove barriers to vaccine access and provide clear guidance to providers, insurers and the public in response to federal actions that the state said restricted vaccine availability.
Nevada’s State Board of Pharmacy updated guidance on Sept. 5 to allow pharmacists to administer the new COVID-19 shot and other FDA-approved vaccines. Several retail pharmacy chains, including CVS, had temporarily paused giving the COVID-19 vaccine in the state but said they would resume after the new guidance.
New Jersey’s health department issued an executive directive and standing order permitting anyone 6 months or older to receive the vaccine and allowing pharmacists to administer it to people 3 years and older without a prescription. State officials said the directive was informed by recommendations from scientific agencies including the American Academy of Pediatrics.
New Mexico’s health department issued a standing order on Sept. 11 permitting pharmacists and other providers to vaccinate people 6 months and older without a physician prescription. “We are clearing the way for New Mexicans who want the vaccine to get the vaccine,” Health Secretary Gina DelBasa said in a statement accompanying the order.
New York Gov. Kathy Hochul signed an executive order on Sept. 5 that declared a state disaster "due to federal actions related to vaccine access" and allowed pharmacists to administer COVID-19 shots to anyone age 3 and older through Oct. 5. The order also authorizes physicians and nurse practitioners to prescribe vaccines that pharmacists may then administer.
Pennsylvania’s State Board of Pharmacy altered its rules to allow pharmacists to administer the COVID-19 shot based on recommendations from authorities other than the federal Advisory Committee on Immunization Practices. The board’s statement said new sources of authority may include organizations such as the American College of Obstetricians and Gynecologists, the American Academy of Pediatrics, the American Academy of Family Physicians and the FDA. Following that decision, CVS said it would resume administering vaccines at locations across the commonwealth.
Virginia’s state health commissioner signed a standing order on Sept. 10 allowing pharmacists to vaccinate people 18 to 64 with underlying health conditions, and anyone 65 and older, without a prescription; the order directs providers to follow the CDC immunization schedule as applied by the state.
On Sept. 3 California, Oregon and Washington formed a West Coast Health Alliance to coordinate public health guidance. In a joint statement the three governors said they would provide coordinated health guidance based on vaccine recommendations from "respected national medical organizations" and vowed to "uphold scientific integrity in public health." The governors also criticized what they described as politicization of federal public health agencies.
Taken together, the state actions reflect growing divergence between federal authorization limits and the policies of many state and professional bodies. Public health officials in the states issuing standing orders and executive directives said their goal is to remove barriers to vaccination, maintain routine immunization services, and allow clinicians and patients to follow medical guidance they view as evidence-based.
The federal FDA authorization restricts the newly updated shots to higher-risk adults, but state officials and medical societies have emphasized broader approaches for children, pregnant people and families concerned about COVID-19. The result is a varied patchwork of access that will depend on state law, the decisions of pharmacy chains and health systems, the stance of insurers and upcoming rulings by state immunization advisory committees.
Health departments and state pharmacy boards said they expected many pharmacies and clinics to resume offering COVID-19 vaccines as standing orders and executive directives took effect. Several states also set deadlines for further public guidance: Illinois officials, for example, required the state health department to publish clear recommendations by Sept. 26 following its advisory committee meeting.
Public health experts have said that consistent messaging and easy access influence vaccine uptake. State leaders enacting broader access measures argued that their steps were intended to preserve that access and to let clinicians and patients make individualized medical decisions consistent with national professional guidance and local circumstances.