Study links high blood pressure at age 7 to greater risk of midlife cardiovascular death; experts urge childhood screening
Researchers say elevated blood pressure in early childhood is associated with up to a 50% higher risk of cardiovascular death over the next five decades, prompting calls for routine checks.
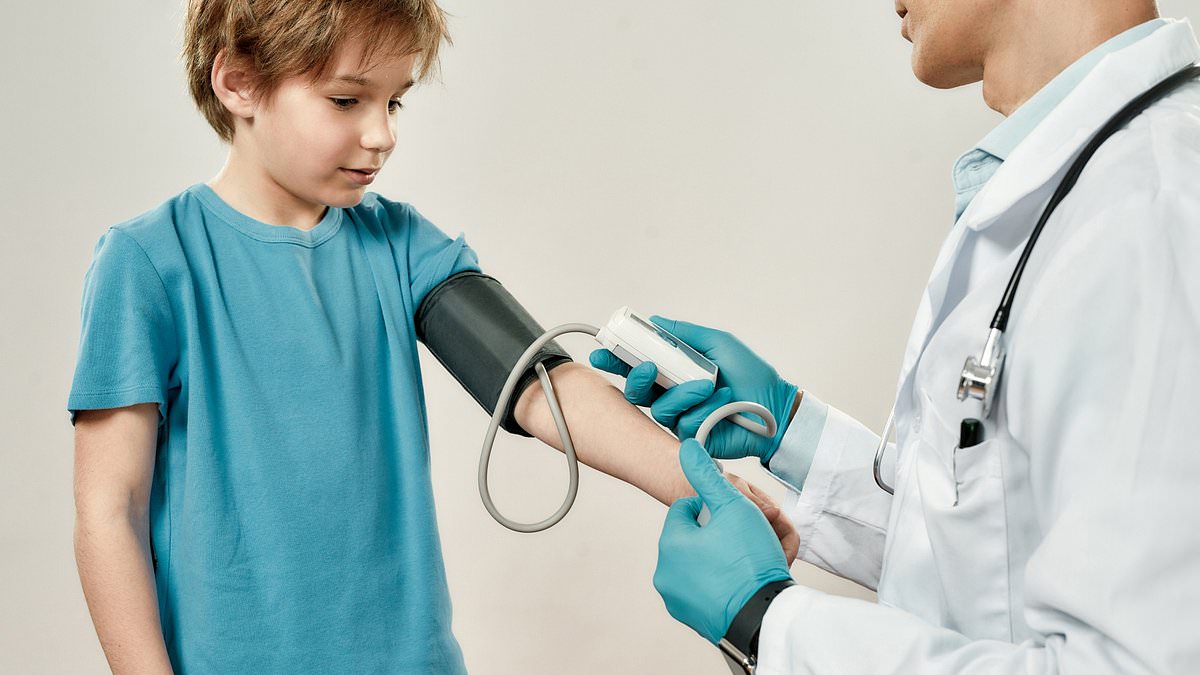
A long-term study has found that children with higher blood pressure at age 7 face a substantially increased risk of dying from cardiovascular disease in midlife, and experts said the findings support routine blood pressure screening in childhood.
Researchers analysed blood pressure measurements taken at age 7 from about 38,000 participants in a long-running U.S. cohort and followed them for an average of 54 years. Children whose readings were in the highest 10 percent for their age, sex and height had the greatest elevation in risk, with lead author Alexa Freedman of Northwestern University saying having hypertension or elevated blood pressure as a child "may increase the risk of death by 40 per cent to 50 per cent over the next five decades of an individual's life." The findings were published in JAMA and presented at the American Heart Association Hypertension Scientific Sessions 2025 in Baltimore.
Freedman and colleagues said their results underscore the potential value of early detection and prevention strategies to promote lifelong cardiovascular health. "Our results highlight the importance of screening for blood pressure in childhood and focusing on strategies to promote optimal cardiovascular health beginning in childhood," she said.
The study builds on prior research that linked elevated blood pressure in older children to higher cardiovascular mortality by mid-adulthood. Investigators noted that blood pressure in childhood tracks into later life for many individuals, and early elevation may contribute to cumulative vascular damage decades before clinical disease becomes apparent.
Clinical guidance differs between countries. The American Academy of Pediatrics recommends measuring blood pressure at annual paediatric visits beginning at age 3. In contrast, the UK National Screening Committee does not currently recommend routine blood pressure screening in children, citing uncertainties about how common childhood hypertension is, limits in the accuracy of screening tests for young people, and unclear evidence on how screening would affect long-term adult disease.
Bonita Falkner, emeritus professor of paediatrics and medicine at Thomas Jefferson University, said the new analysis "supports monitoring blood pressure as an important metric of cardiovascular health in childhood." She added that attention to blood pressure alongside other risk factors could inform early prevention.
High blood pressure, or hypertension, typically causes no symptoms but increases the risk of heart attacks, strokes, heart failure and other serious conditions if left untreated. Adult thresholds commonly used to define hypertension are 140/90 mmHg or higher, but blood pressure evaluation in children is based on percentiles that account for age, sex and height. The study emphasised that children in the top decile for these adjusted measurements were at the highest risk of later cardiovascular death.
Public health authorities say many adults with hypertension are unaware of their condition. In the UK, more than one in four adults are estimated to have high blood pressure, according to National Health Service figures. Study authors and some clinicians argue that identifying elevated blood pressure earlier in life could allow families and health services to encourage heart-healthy behaviours, treat underlying conditions when appropriate, and potentially reduce midlife cardiovascular mortality.
The investigators cautioned that screening programmes should be accompanied by validated measurement methods and clear pathways for follow-up, diagnosis and management. The UK screening committee has previously highlighted questions about measurement accuracy in children and the availability of evidence on effective interventions starting in childhood.
The new analysis used archived blood pressure readings and long-term mortality records to examine associations, and authors stressed that observational data cannot by itself prove that screening and early intervention will reduce deaths. Nevertheless, they and other experts said the size of the association over a half-century of follow-up adds to a growing evidence base linking childhood cardiovascular risk markers with adult disease.
Clinicians and parents are advised to be aware of blood pressure as one component of cardiovascular risk assessment and to follow national guidance on screening and management. Further research, including studies of screening implementation, standardised measurement techniques and the effectiveness of early interventions, will be needed to determine optimal policy approaches in different health systems.