Study links missed first breast cancer screening to higher long-term mortality
Researchers say skipping the initial mammogram is associated with later-stage diagnosis and lower future screening uptake, with potential policy implications for UK programs
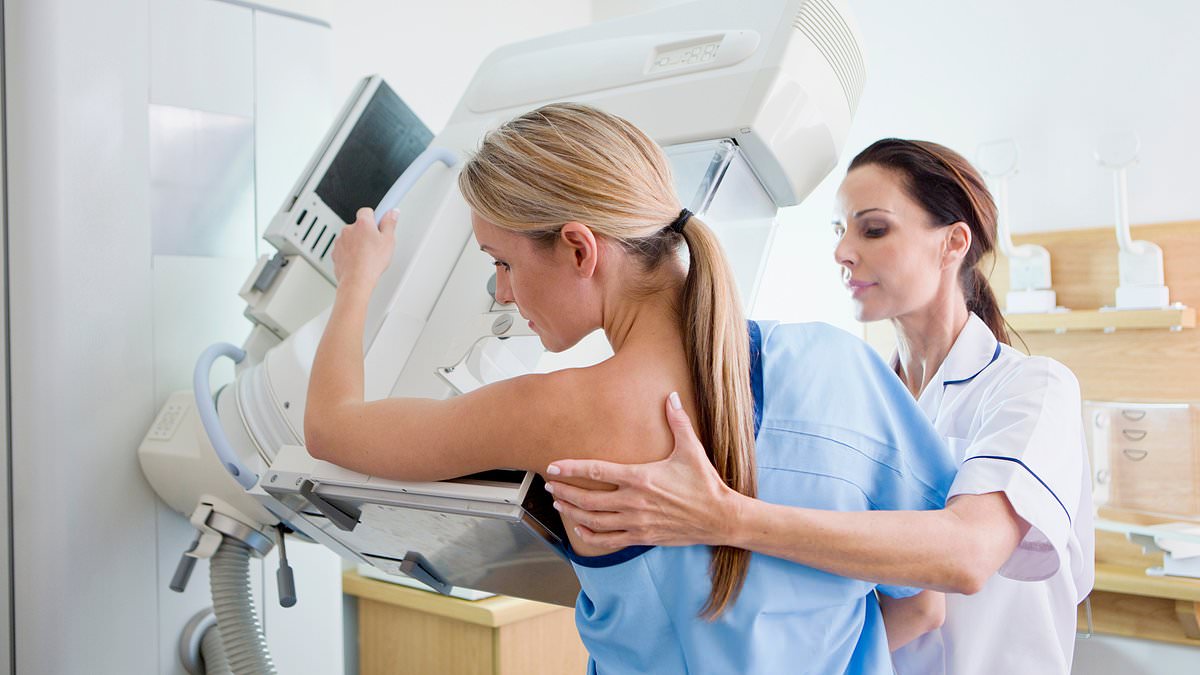
A Swedish study has found that women who miss their first breast cancer screening appointment face a substantially higher risk of dying from the disease over the next 25 years. After following nearly half a million women who were invited to screening between 1991 and 2020, researchers report a 40 per cent higher risk of breast cancer mortality for those who did not attend their first mammogram, even after adjusting for a range of social, economic, reproductive, and health-related factors. The study also shows that women who skip their first screening are less likely to attend future invitations, and they are more likely to be diagnosed with cancer at an advanced stage than those who participate.
The researchers analyzed data for about 490,000 women who received their first screening invitation in Sweden over a nearly 30-year span and were followed for up to 25 years. They found that 32 per cent did not attend their initial mammogram. Those who did not attend were also less likely to participate in subsequent screenings and more likely to be diagnosed at a more advanced stage. Mortality data showed 9.9 breast cancer deaths per 1,000 women over 25 years among non-attenders, compared with 7 per 1,000 among attenders. By contrast, the 25-year incidence of breast cancer was similar between the two groups, suggesting that the higher death rate among non-attenders reflects delayed detection rather than a higher underlying risk.
"First screening non-participants had a 40 per cent higher breast cancer mortality risk than participants, persisting over 25 years," the study authors wrote in the British Medical Journal. They added that the increased mortality is largely due to delayed detection and that the first mammography screening could be a crucial window for preventing adverse outcomes. The findings align with the idea that early detection improves survival and that patterns of engagement with screening may forecast future cancer trajectories.
The study comes as health officials in the United Kingdom weigh how to maximize screening uptake. In England, women are invited for breast screening from age 50 to 71, with the first invitation typically arriving by age 53. NHS data show that as of March 2024, about 70 per cent of eligible women were up to date with breast screening, leaving roughly one in three not up to date. Scotland and Wales offer routine screening to women aged 50 to 70. Mammograms can detect breast cancer early, often before a lump is felt, and early detection is associated with higher survival rates.
Claire Rowney, chief executive of the charity Breast Cancer Now, said that despite screening being the most effective way to find cancer early, thousands of UK women still miss this vital check. She noted that those who miss their first appointment are far less likely to participate in future screenings and urged governments across the UK to push toward the target of 80 per cent uptake. "Maximising the number of women attending breast screening will be a game changer in helping to ensure more breast cancers are diagnosed early and more lives are saved from this devastating disease," Rowney said.
US researchers who wrote a companion commentary to the study emphasized that the decision to attend the first screening is not just about a one-off health check; it represents a long-term investment in breast health and survival. The new findings underscore the potential value of identifying populations at higher risk for late presentation decades before adverse outcomes occur and tailoring outreach to improve initial attendance and ongoing engagement with screening programs.
The Swedish analysis adds to a growing body of evidence suggesting that initial engagement with breast screening has lasting implications for outcomes. While the overall incidence of breast cancer may be similar over long follow-up, the timing of detection appears central to survival. Researchers cautioned that the study, while robust, reflects data from a single country and healthcare system, and they call for additional work to understand how these findings translate across different settings and to explore targeted strategies that encourage first attendance and continued participation. In the meantime, public health advocates stress the importance of making screening accessible and acceptable to all eligible women, with clear barriers to attendance addressed through outreach, scheduling flexibility, and community-based support.
If health systems can convert first-appointment attendees into sustained screen participants, experts say, the effect could extend beyond individual lives to overall population outcomes, helping to shift detection toward earlier stages when treatment is most effective. As policymakers consider how to lift uptake toward the 80 per cent goal, the study offers a stark reminder that missing that initial invitation may carry consequences far beyond the immediate health check.