UK trial offers blood test to improve Alzheimer's diagnosis
More than 1,000 people with suspected dementia will be recruited across 20 memory clinics to test a p‑tau217 blood biomarker that could boost diagnostic accuracy and speed.
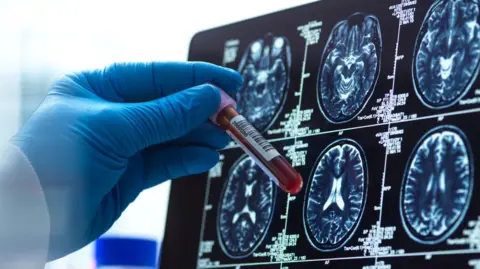
More than 1,000 people across the UK with suspected dementia are to be offered a blood test that researchers say could substantially improve and speed up diagnosis of Alzheimer's disease.
The Alzheimer's Disease Diagnosis and Plasma p‑tau217 (ADAPT) trial, led by University College London, will recruit patients at 20 memory clinics to evaluate a blood biomarker called p‑tau217 alongside standard cognitive assessments. Scientists running the study said the test, which costs about £100, measures a form of tau protein associated with the amyloid and tau deposits that define Alzheimer's and could raise diagnostic accuracy from roughly 70% to more than 90%.
The trial began recruitment at a memory clinic in Essex, with 19 additional NHS centres planned. Half of participants will receive their blood test results within three months and the remainder after 12 months. Investigators will compare the groups to determine whether earlier test results speed diagnosis, change decisions about further investigation such as PET scans or lumbar punctures, and affect how patients and clinicians interpret and act on findings.
Alzheimer's disease, the most common form of dementia, is characterised by the build-up of amyloid and tau proteins in the brain, processes that can begin up to two decades before symptoms arise. Until recently, confirmation of the disease relied on specialist PET brain imaging or analysis of cerebrospinal fluid obtained by lumbar puncture. Those procedures are not part of routine diagnosis in the NHS, and only about 2% of patients currently undergo them.
Professor Jonathan Schott, professor of neurology at UCL and chief medical officer at Alzheimer's Research UK, said the ADAPT study was "a critical part of the Blood Biomarker Challenge, which we hope will take us a step forward in revolutionising the way we diagnose dementia." The trial is supported by Alzheimer's Research UK and the Alzheimer's Society and has funding from the People's Postcode Lottery.

Professor Fiona Carragher, chief policy and research officer at the Alzheimer's Society, pointed to shortcomings in current diagnosis pathways. She said a recent survey of people with lived experience showed only a third regarded their diagnosis experience as positive, and that many reported fear of receiving a diagnosis. "As a result, too often, dementia is diagnosed late, limiting access to support, treatment and opportunities to plan ahead," she said.
The ADAPT trial will also measure the impact of receiving a blood test result on patients' quality of life. Investigators will track whether knowledge of biomarker status influences emotional wellbeing, use of services, and uptake of further investigations or treatments. Results of the trial are expected in about three years.
Patient advocates involved in designing the study said the test could change how families and clinicians approach Alzheimer's. Steven Pidwell, 71, whose partner Rachel Hawley was diagnosed with Alzheimer's nearly a decade ago, described an accurate, rapid blood test combined with emerging treatments as a "gamechanger" for families. The couple, who were among volunteers with lived experience consulted by UCL researchers, said an earlier, clearer diagnosis could allow better planning and normalise living with the condition.
The p‑tau217 blood test detects a phosphorylated form of the tau protein that researchers say reflects the presence of both tau and amyloid pathology in the brain. Several research groups have reported that measures of p‑tau217 in plasma correlate well with PET imaging and cerebrospinal fluid markers, but most evidence to date has come from specialised research settings rather than routine clinical practice.
If ADAPT shows that adding the blood test to current assessment pathways improves diagnostic accuracy, reduces time to diagnosis, or helps clinicians make better-informed decisions about further testing and care, it could be considered for wider use in the NHS. That prospect has taken on added urgency as a number of therapies targeting early-stage Alzheimer's are in the late stages of clinical development; accurate early diagnosis would be important for identifying people who might benefit from such treatments.
The trial will not replace PET scans or lumbar punctures where they are clinically indicated, but its designers hope a low‑cost, minimally invasive blood test could make biochemical assessment of Alzheimer's more accessible across the health service. The ADAPT team emphasised that the trial has ethical safeguards and that participants will receive support and information as part of routine memory clinic care.
UCL researchers expect that if the trial meets its goals, more widespread adoption of plasma biomarkers could change diagnostic pathways in primary and secondary care over the coming years. For now, the study will test whether the promise seen in research centres translates to benefit for patients, clinicians and the NHS in real-world clinical settings.
