William Harvey Hospital uses Costa Café as makeshift ward amid bed shortages
Campaigners call arrangement humiliating as hospital faces criticism over corridor care and wider NHS funding pressures
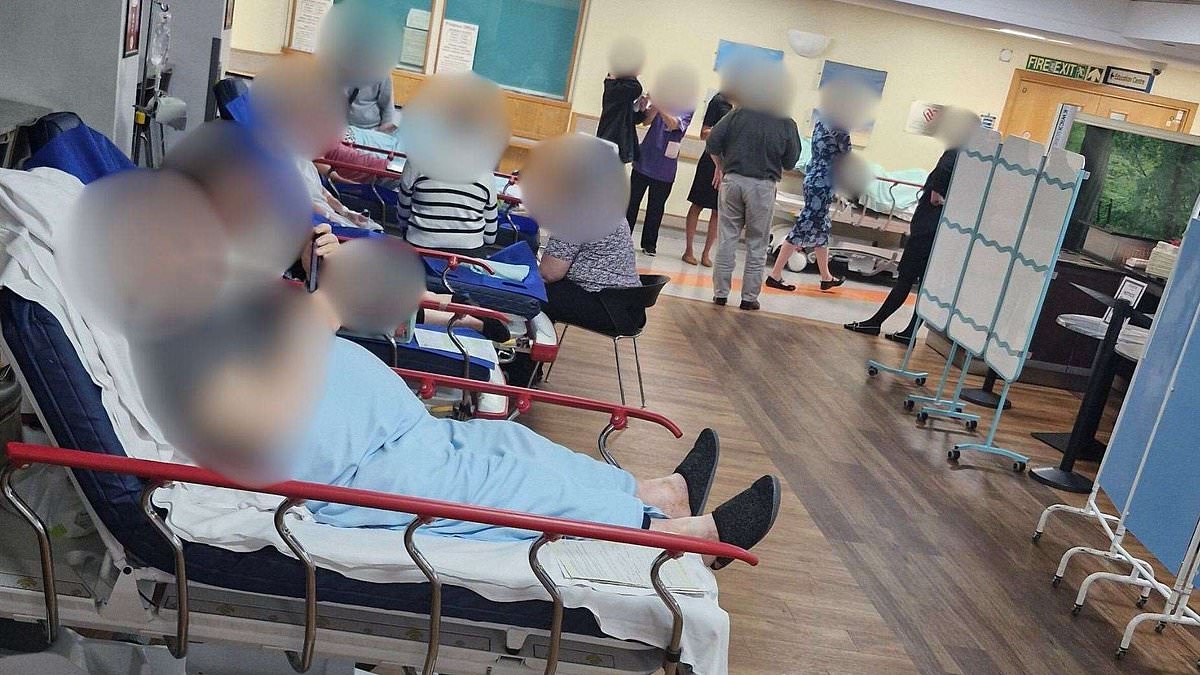
An overwhelmed hospital in Ashford has turned its Costa Café into a makeshift ward to cope with severe bed shortages, a move health campaigners branded as humiliating. Images circulating this week show elderly patients lying on beds wheeled into the Costa Coffee branch at William Harvey Hospital, part of the East Kent Hospitals Trust.
An anonymous relative of a patient held at the hospital described the scene as a failure of care, telling reporters that staff were doing what they could but there was simply no space left. “Leaving people to rot,” she said, adding that the arrangement raises questions about how the elderly are treated when wards and corridors are full and non-clinical areas are used for patient care. The relative urged others with loved ones at the hospital to be concerned about the message this sends about the state of hospital care.
Ken Rogers, chair of Concern for Health in East Kent, called the makeshift ward horrendous and said it is absolutely disgusting for patients to be treated this way. He noted that beds being shuffled into a cafe simply because there is no space on wards or in corridors demonstrates the severity of the bed shortage in the region and urged East Kent Hospitals to press for more resources and support from national authorities.
The controversy comes as the East Kent Hospitals Trust, which also runs the QEQM hospital in Margate, faces ongoing scrutiny of its performance. A national league table released last week placed East Kent 101st out of 134 acute care providers. In August, 1,311 people waited for at least 12 hours for a bed—a rise of 116 from the same month last year and the third-highest figure in England.
Experts say bed-blocking—the situation where patients who are well enough to leave cannot be discharged due to a lack of appropriate care packages or placements—has contributed to longer waits in emergency departments and a rise in what some describe as corridor care, where treatment spills into hallways. Ashford MP Sojan Joseph described corridor care as an unfortunate and unacceptable consequence of a decade and a half of NHS cuts, pledging to push for changes that move care away from hospitals toward community-based solutions. He noted that the government’s 10-Year Health Plan for England recognizes the need to re-balance services toward local, community-focused care.
As part of that shift, Folkestone and Hythe has been named one of six pioneer sites in the South East for the Neighbourhood Health Programme. The national scheme aims to integrate medical and social care with local government and charity partners to support people with long-term conditions. Earlier pilots in Folkestone and Hythe showed promising results, with at-risk patients’ A&E attendance dropping from 223 to 33 within six months at one scheme. The project is funded with up to £10 million in national money, with NHS leaders hoping such efforts will ease hospital pressures by addressing problems earlier and closer to where people live.
Meanwhile, the tragedy surrounding Dorothy Reid, a 91-year-old who died after a lengthy wait at another hospital, has intensified concern about bed-blocking and lengthy A&E waits. North East Kent Coroner Catherine Wood concluded that Mrs. Reid might not have died had she visited the hospital earlier, describing the issue as a national crisis rather than a local one and warning that there is a risk of future deaths unless action is taken to tackle bed-blocking and long waits.
A Department of Health and Social Care spokesperson said: “This is unacceptable and we expect the William Harvey Hospital to take urgent action to address this. All NHS trusts should provide safe, dignified care in appropriate clinical settings. We inherited an emergency care system on its knees, but we are working at pace to turn the tide on more than a decade of neglect and improve care for patients. We are also strengthening plans to winter-proof our NHS, from war-game exercises to extra checks for the most vulnerable, to ease pressure on hospitals and ensure patients get the care they need.” East Kent Hospitals was approached for comment.